Topic
- Anterior cerebral artery
- Anterior Choroidal Artery
- Anterior Communicating Artery
- Anterior temporal artery anatomy
- Anterolateral central (lenticulostriate) arteries anatomy
- Anteromedial central (perforating) arteries anatomy
- Artery of central sulcus
- Artery of postcentral sulcus
- Artery of precentral sulcus
- Artery to angular gyrus anatomy
- Basilar artery
- Callosomarginal artery
- Inferior hypophyseal artery anatomy
- Internal carotid artery
- Labyrinthine artery
- Lateral frontobasal artery
- Long medial striate artery
- Medial frontobasal artery
- Middle cerebral artery
- Middle temporal artery
- Ophthalmic artery
- Paracentral artery
- Pericallosal artery
- Polar frontal artery
- Polar temporal artery
- Pontine arteries
- Posterior cerebral artery
- Posterior communicating artery
- Posterior lateral choroidal artery
- Posterior parietal artery
- Posteromedial central (perforating) arteries
- Precuneal artery
- Superior cerebellar artery
- Superior hypophyseal artery
- Anterior lobe of cerebellum
- Anterior quadrangular lobule
- Arbor Vitae (Cerebellar White Matter)
- Central lobule
- Cerebellar commissure
- Cerebellar tentorium
- Cerebellopontine angle
- Cerebellum
- Culmen
- Declive
- Dentate nucleus
- Flocculonodular lobe
- Folium of Vermis
- Horizontal fissure (cerebellum)
- Inferior cerebellar peduncle
- Inferior semilunar lobule
- Intraculminate fissure
- Lingula of cerebellum
- Lunogracle fissure
- Middle cerebellar peduncle
- Nodule of vermis
- Paramedian lobule
- Posterior lobe of cerebellum
- Posterior superior fissure
- Posterolateral fissure
- Prebiventral fissure
- Precentral fissure
- Preculminate fissure
- Primary fissure
- Pyramis of vermis
- Secondary fissure
- Simple lobule
- Superior medullary velum
- Superior semilunar lobule of cerebellum
- Tonsil of cerebellum
- Tuber of vermis
- Uvula of vermis
- Wing of central lobule
- Ambient cistern
- Carotid cistern
- Chiasmatic cistern
- Cistern of central sulcus
- Cistern of lamina terminalis
- Cistern of lateral cerebral fossa
- Cistern of transverse fissure
- Crural cistern
- Interpeduncular Cistern
- Lateral cerebellomedullary cistern
- Oculomotor cistern
- Olfactory cistern
- Pericallosal cistern
- Pontocerebellar cistern
- Posterior cerebellomedullary cistern (cisterna magna)
- Prepontine cistern
- Quadrigeminal cistern
- Superior cerebellar cistern
- Abducens nerve (Cranial nerve VI)
- Accessory Nerve (Cranial nerve XI)
- Cochlea
- Cochlear nerve (Cranial nerve VIII)
- Facial Nerve (Cranial nerve VII)
- Glossopharyngeal nerve (Cranial nerve IX)
- Hypoglossal Nerve (Cranial nerve XII)
- Inferior branch vestibular nerve
- Inferior salivatory nucleus
- Inferior vestibular nucleus
- Lacrimal nucleus
- Lateral vestibular nucleus
- Medial vestibular nucleus
- Mesencephalic nucleus of trigeminal nerve
- Motor nucleus of facial nerve
- Motor nucleus of trigeminal nerve
- Nucleus of abducens nerve
- Nucleus of hypoglossal nerve
- Nucleus of oculomotor nerve
- Nucleus of solitary tract
- Nucleus of trochlear nerve
- Oculomotor Nerve (Cranial Nerve III)
- Olfactory bulb
- Olfactory Nerve (Cranial Nerve I)
- Olfactory tract
- Optic chiasm
- Optic Nerve (Cranial Nerve II)
- Posterior cochlear nucleus
- Principal sensory nucleus of the trigeminal nerve
- Semicircular Canals
- Spinal nucleus of trigeminal nerve
- Superior branch of vestibular nerve
- Superior salivatory nucleus
- Superior vestibular nucleus
- Trigeminal ganglion
- Trigeminal nerve (Cranial nerve V)
- Trochlear nerve (Cranial nerve IV)
- Vagus nerve (Cranial nerve X)
- Vestibular ganglion
- Vestibule
- Vestibulocochlear nerve (Cranial nerve VIII)
- Anterior cochlear nucleus
- Angular gyrus
- Anterior long insular gyrus
- Anterior orbital gyrus
- Anterior short insular gyrus
- Cingulate gyrus
- Cuneus
- Descending occipital gyrus
- Frontal operculum
- Frontal pole
- Inferior frontal gyrus
- Inferior occipital gyrus
- Inferior temporal gyrus
- Insular cortex
- Lateral occipitotemporal gyrus
- Lateral orbital gyrus
- Lingual gyrus
- Long gyri of insula
- Medial frontal gyrus
- Medial occipitotemporal gyrus
- Medial orbital gyrus
- Middle frontal gyrus
- Middle occipital gyrus
- Middle short insular gyrus
- Middle temporal gyrus
- Occipital pole
- Parahippocampal gyrus
- Paraterminal gyrus
- Pars opercularis of inferior frontal gyrus
- Pars orbitalis of inferior frontal gyrus
- Pars triangularis of inferior frontal gyrus
- Postcentral gyrus
- Posterior long insular gyrus
- Posterior orbital gyrus
- Posterior short insular gyrus
- Precentral gyrus
- Precuneus
- Short gyri of insula
- Straight gyrus
- Superior frontal gyrus
- Superior occipital gyrus
- Superior parietal lobule
- Superior temporal gyrus
- Supramarginal gyrus
- Temporal pole
- Transverse temporal gyri
- Alveus
- Amygdala
- Choroid plexus of lateral ventricle
- Cornu Ammonis 1 (CA1)
- Cornu ammonis 2 (CA2)
- Cornu ammonis 3 (CA3)
- Cornu ammonis 4 (CA4)
- Cornu ammonis
- Dentate gyrus
- Fimbria of hippocampus
- Hippocampal body
- Hippocampal head
- Hippocampal tail
- Parasubiculum (Presubiculum)
- Posterior medial choroidal artery
- Prosubiculum
- Subiculum
- Uncus
- Vestigial hippocampal sulcus
- Aqueduct of midbrain (Sylvian Aqueduct)
- Brachium of inferior colliculus
- Brachium of superior colliculus
- Cerebral crus
- Decussation of the superior cerebellar peduncles
- Inferior colliculus
- Inferior olive
- Lateral longitudinal fasciculus
- Medial longitudinal fasciculus
- Medulla oblongata
- Pons
- Pontine nucleus
- Pyramids of the medulla oblongata
- Red nucleus
- Substantia nigra
- Superior colliculus
- Tegmentum of midbrain
- Anterior commissure
- Anterior intercavernous sinus
- Anterior limb of internal capsule
- Anterior lobe of pituitary gland
- Body of caudate nucleus
- Body of corpus callosum
- Body of fornix
- Calcarine spur
- Caudato-lenticular bridges
- Cave of septum pellucidum
- Central canal
- Choroid plexus of fourth ventricle
- Claustrum
- Column of fornix
- Corona radiata
- Corticospinal tract
- Crus of fornix
- External capsule
- Foramen caecum of medulla oblongata
- Frenulum veli
- Genu of corpus callosum
- genu of internal capsule
- Globus pallidus external segment
- Globus pallidus internal segment
- Habenular commissure
- Head of caudate nucleus
- Inferior opening of cerebral aqueduct
- Insular threshold
- Internal medullary lamina
- Interpeduncular fossa
- Interthalamic adhesion
- Isthmus of cingulate gyrus
- Lamina terminalis
- Lateral geniculate body
- Limbic lobe
- Mammillary body
- Medial geniculate body
- Optic tract
- Pineal recess
- Pituitary gland
- Pituitary stalk
- Posterior commissure
- Posterior intercavernous sinus
- Posterior limb of internal capsule
- Posterior lobe pituitary gland
- Preoptic area
- Pulvinar
- Putamen
- Raphe of pons
- Rostrum of corpus callosum
- Septum pellucidum
- Upper cervical spinal cord
- Splenium of corpus callosum
- Superior opening of the cerebral aqueduct
- Suprapineal recess
- Tail of caudate nucleus
- Thalamus
- Transverse pontine fiber
- Trigeminal cave
- Tuber cinereum
- Anterior ascending ramus of Sylvian fissure
- Anterior horizontal ramus of Sylvian fissure
- Anterior median fissure of medulla oblongata
- Basilar sulcus
- Calcarine Sulcus
- Central sulcus
- Central sulcus of insula
- Cingulate sulcus
- Circular sulcus of insula
- Collateral sulcus
- Hippocampal sulcus
- Inferior frontal sulcus
- Inferior temporal sulcus
- Intraparietal sulcus
- Lateral sulcus (Sylvian fissure)
- Longitudinal cerebral fissure
- Marginal sulcus
- Median sulcus of the 4th ventricle
- Occipitotemporal sulcus
- Olfactory sulcus
- Para-brachial recess
- Paracentral sulcus
- Parietooccipital sulcus
- Pontomedullary sulcus
- Postcentral sulcus
- Posterior ramus of lateral sulcus
- Post-olivary sulcus
- Precentral sulcus
- Pre-olivary sulcus
- Rhinal sulcus
- Subparietal sulcus
- Sulcus of corpus callosum
- Superior frontal sulcus
- Superior temporal sulcus
- Ventrolateral sulcus of medulla oblongata
- Anterior cerebral veins
- Anterior vein of caudate nucleus
- Anterolateral medullary vein
- Anteromedian medullary vein
- Anteromedian pontine vein
- Basal vein of rosenthal
- Basilar plexus
- cavernous sinus
- Confluence of sinuses
- Deep mddle cerebral veins
- Diploic veins
- Dorsal vein of corpus callosum
- Frontal veins
- Frontopolar vein
- Great cerebral vein
- Inferior anastomotic vein (Vein of Labbé)
- Inferior hemispheric veins of the cerebellum
- Inferior petrosal sinus
- Inferior sagittal sinus
- Inferior vein of vermis
- Internal cerebral vein
- Internal jugular vein
- interpeduncular veins
- Lateral mesencephalic vein
- Lateral pontine vein
- Lateral vein of lateral ventricle
- Marginal sinus
- Mastoid emissary vein
- Occipital emissary vein
- Occipital sinus
- Occipital veins
- Parietal veins
- Petrosal vein
- Posterior mesencephalic vein
- Posterior vein of caudate nucleus
- Posterior veins of septum pellucidum
- Posteromedian medullary vein
- Precentral cerebellar vein
- Sigmoid sinus
- Straight sinus
- Superficial cerebral veins
- Superficial middle cerebral vein
- Superior anastomotic vein
- Superior cerebellar vein
- Superior hemispheric veins of the cerebellum
- Superior petrosal sinus
- Superior sagittal sinus
- Superior thalamic veins
- Superior thalamostriate vein
- Superior vein of vermis
- Transverse sinus
- Transverse veins of caudate nucleus
- Vein of lateral recess of fourth ventricle
- Vein of septum pellucidum
- Venous plexus of foramen ovale
- Venous plexus of hypoglossal canal
- Atrium of lateral ventricle
- Central part of lateral ventricle
- Fourth ventricle
- Frontal horn of lateral ventricle
- Infundibular recess
- Interventricular foramen
- Lateral aperture of the fourth ventricle
- Lateral recess fourth ventricle
- Median aperture of the fourth ventricle
- Obex
- Occipital horn of lateral ventricle
- Supraoptic recess
- Temporal horn of lateral ventricle
- Third ventricle
- Anterior Band of Articular Disc TMJ
- Posterior band of articular disc, TMJ
- Articular capsule of temporomandibular joint
- Articular disc of temporomandibular joint
- Articular eminence
- Articular surface of mandibular fossa
- Articular tubercle
- Attachment of inferior head of lateral pterygoid muscle
- Attachment of superior head of lateral pterygoid muscle
- Auricle (Pinna)
- External acoustic meatus
- Glenoid process of parotid gland
- Intermediate zone of articular disc
- Lateral temporomandibular ligament
- Parotid gland
- Superior retrodiscal layer
- Superior synovial membrane of temporomandibular joint
- Temporomandibular joint
- Mandible
- Mandibular condyle
- Mandibular fossa
- Mastoid process
- Neck of mandible
- Petrous part of temporal bone
- Ramus of mandible
- Sheath of styloid process
- Squamous part of temporal bone
- Styloid process
- Tympanic part of temporal bone
- Zygomatic process of temporal bone
- Deep part of masseter muscle
- Superficial part of masseter
- Superior head of lateral pterygoid muscle
- Inferior head of lateral pterygoid muscle
- Lateral pterygoid muscle
- Masseter muscle
- Medial pterygoid muscle
- Temporalis muscle
- Auriculotemporal nerve
- Maxillary veins
- Transverse facial vein
- Transverse facial artery
- Pterygoid venous plexus
- Tragus of ear
- Crus helix of ear
- Superficial temporal vein
- Posterior auricular vein
- Retromandibular vein
- Superficial temporal artery
- Oculomotor nerve (Superior branch)
- Oculomotor nerve (inferior branch)
- Abducens nerve (orbital part )
- Maxillary nerve
- Intracranial part of optic nerve
- Frontal nerve
- Superior rectus muscle
- Superior ophthalmic vein
- Lacrimal artery
- Lateral rectus muscle
- Inferior ophthalmic vein
- Zygomatic nerve
- Levator palpebrae superioris muscle
- Superior oblique muscle
- Medial rectus muscle
- Orbital part of optic nerve
- Retrobulbar fat
- Inferior rectus muscle
- Infraorbital nerve
- Optic nerve sheath
- Subarachnoid space of optic nerve
- Common tendinous ring (Annulus of zinn)
- Optic canal
- Superior eyelid
- Inferior eyelid
- Superior tarsus
- Inferior tarsus
- Inferior oblique muscle
- Orbicularis oculi muscle
- Lacrimal gland
- Lacrimal nerve
- Lacrimal vein
- Lacrimal canaliculi
- lens of the eye
- Cornea
- Iris
- Pupil
- Anterior chamber of eyeball
- Posterior chamber of eyeball
- Vitreous chamber of eyeball
- Sclera
- Choroid
- Retina
- Nasolacrimal duct (Tear duct)
- Supratrochlear vein
- Supratrochlear nerve
- Supratrochlear artery
- Supraorbital nerve
- Supraorbital artery
- Supraorbital vein
- Optic disc
- Nasofrontal vein
- Whitnall's ligament
- Lockwood’s ligament
- Lateral canthal ligament
- Medial canthal ligament
- Brachiocephalic trunk
- Carotid bifurcation
- Common carotid artery
- External carotid artery
- Facial artery
- Inferior thyroid artery
- Internal carotid artery (cavernous part)
- Internal carotid artery (cervical part)
- Internal carotid artery (petrous part)
- Subclavian artery
- Left subclavian artery
- Right subclavian artery
- Lingual artery
- Maxillary artery
- Posterior auricular artery
- Transverse cervical artery
- Anterior jugular vein
- External jugular vein
- Facial vein
- Submental vein
- Superior bulb of internal jugular vein
- Cervical spinal nerve 1 (C1)
- Cervical spinal nerve 2 (C2)
- Cervical spinal nerve 3 (C3)
- Cervical spinal nerve 4 (C4)
- Cervical spinal nerve 5 (C5)
- Cervical spinal nerve 6 (C6)
- Cervical spinal nerve 7 (C7)
- Cervical spinal nerve 8 (C8)
- Mandibular canal
- inferior alveolar artery
- Inferior alveolar nerve
- Mental nerve
- Auricularis anterior muscle
- Auricularis posterior muscle
- Buccinator muscle
- Depressor anguli oris muscle
- Depressor labii inferioris muscle
- Depressor septi nasi muscle
- Hyoglossus muscle
- Cricothyroid muscle
- Hyoglossus
- Iliocostalis cervicis muscle
- Inferior belly of omohyoid muscle
- Inferior longitudinal lingual muscle
- Lateral cricoarytenoid muscle
- Levator anguli oris muscle
- Levator labii superioris alaeque nasi muscle
- Levator labii superioris muscle
- Superior longitudinal muscle of tongue
- Inferior longitudinal muscle of tongue
- Transverse muscle of the tongue
- Longissimus capitis muscle
- Longissimus cervicis muscle
- Longus capitis muscle
- Longus colli muscle
- Masseter muscle (Deep part)
- Masseter muscle (Superficial part)
- Superficial head of medial pterygoid muscle
- Mentalis muscle
- Middle constrictor muscle of pharynx
- Multifidus muscles
- Mylohyoid muscle
- Nasalis muscle
- Obliquus inferior capitis muscle
- Obliquus superior capitis muscle
- Orbicularis oculi muscle (Orbital part)
- Orbicularis oculi muscle (Preseptal part)
- Orbicularis oris muscle
- Palatoglossus muscle
- Palatopharyngeus muscle
- Pectoralis major muscle
- Platysma muscle
- Posterior belly of digastric muscle
- Anterior belly of digastric muscle
- Posterior cricoarytenoid muscle
- Rectus capitis anterior muscle
- Rectus capitis lateralis muscle
- Rectus capitis posterior major muscle
- Rectus capitis posterior minor muscle
- Rhomboid major muscle
- Rhomboid minor muscle
- Risorius muscle
- Rotatores cervicis muscle
- Scalenus anterior muscle (Anterior scalene muscle)
- Scalenus posterior muscle (Posterior scalene muscle)
- Scalenus medius muscle (middle scalene muscle)
- Semispinalis capitis muscle
- Semispinalis cervicis muscle
- Serratus anterior muscle
- Serratus posterior superior muscle
- Splenius capitis muscle
- Splenius cervicis muscle
- Spinalis cervicis muscle
- Sternocleidomastoid muscle
- Sternohyoid muscle
- Sternothyroid muscle
- Styloglossus muscle
- Stylopharyngeus muscle
- Stylohyoid muscle
- Subclavius muscle
- Superior belly of omohyoid muscle
- Superior constrictor muscle of pharynx
- Superior longitudinal lingual muscle
- Supraspinatus muscle
- Temporalis muscle (face)
- Tensor veli palatini muscle
- Levator veli palatini muscle
- Thyroarytenoid muscle
- Thyrohyoid muscle
- Transverse arytenoid muscle
- Oblique arytenoid muscle
- Transverse muscle of tongue
- Trapezius muscle
- Vocalis muscle
- Zygomaticus major muscle
- Zygomaticus minor muscle
- Anterior atlanto-occipital membrane
- Aryepiglottic fold
- Auditory tube
- Buccopharyngeal fascia
- Carotid canal
- Cervical part of esophagus
- Choana
- Clivus
- Common nasal meatus
- Conus elasticus
- Cruciate ligament of the atlas
- Dorsum of nose
- Epiglottic vallecula
- Epiglottis
- Foramen cecum of tongue
- Glottis
- Gum (gingiva)
- Hyoepiglottic ligament
- Incisive duct
- Infraglottic cavity
- Intracanalicular part of optic nerve
- Jugular foramen
- jugular foramen pars nervosa
- Jugular foramen pars vascularis
- Laryngeal inlet
- Laryngeal ventricle
- Laryngeal vestibule
- Laryngopharynx
- Lateral glossoepiglottic fold
- Lingual Septum
- Lingual tonsil
- Lower lip
- Median glossoepiglottic fold
- Meckel’s cave (Trigeminal cave)
- Mental foramen
- Nasal vestibule
- Nasopharynx
- Nuchal ligament
- Opening of nasolacrimal duct
- Oropharynx
- Orbital part of orbicularis oculi muscle
- Palatine glands
- Palatine tonsil
- Parotid duct
- Posterior atlanto-occipital ligament
- Preseptal part of orbicularis oculi muscle
- Pterygomandibular raphe
- Root of tongue
- Salpingopalatine fold
- Salpingopharyngeal fold
- Spinal cord
- Sublingual gland
- Submandibular duct
- Submandibular gland
- Tectorial Membrane
- Thyrohyoid membrane
- Thyroepiglottic ligament
- Tonsillar fossa
- Uvula of palate
- Vestibular fold & vestibular ligament
- Anterior arch of atlas
- Anterior nasal spine
- Arch of cricoid cartilage
- Arytenoid cartilage
- Body of hyoid bone
- Body of mandible
- Central inferior incisor tooth
- Central superior incisor tooth
- Clavicle
- Condylar canal
- Costotransverse joint
- Cricoid cartilage
- Dens of axis
- External occipital protuberance
- First rib
- Foramen ovale
- Foramen spinosum
- Frontal process (zygomatic bone)
- Greater alar cartilage
- Greater horn of hyoid bone
- Greater wing of sphenoid bone
- Hyoid bone
- Inferior alveolar foramen (mandibular foramen)
- Inferior canine tooth
- Inferior cornu of thyroid cartilage
- Inferior first premolar tooth
- Inferior second molar tooth
- Inferior second premolar tooth
- Inferior third molar tooth
- Lateral inferior incisor tooth
- Lateral superior incisor tooth
- superior canine tooth
- Superior first molar tooth
- Superior first premolar tooth
- Superior second molar tooth
- Superior second premolar tooth
- Superior third molar tooth
- Inferior nasal concha
- Inferior orbital fissure
- Lamina of cricoid cartilage
- Lamina of thyroid cartilage
- Lateral mass of atlas
- Margin of tongue
- Maxilla
- Maxillary sinus
- Median atlantoaxial joint
- Middle nasal concha
- Nasal septum
- Occipital bone
- Occipital condyle
- Orbital plate
- Orbital surface of maxilla
- Palatine process of maxilla
- Posterior arch of atlas
- Scapula
- Sella turcica
- Superior cornu of thyroid cartilage
- Superior nasal concha
- Thyroid cartilage
- Vomer
- Zygomatic arch
- Zygomatic bone
- Posterior superior alveolar nerve
- Anterior superior alveolar nerve
- Middle superior alveolar nerve
- Mandibular foramen
- Root of lower molar tooth
- Lower molar apical foramen
- Upper premolar apical foramen
- Root of upper molar tooth
- Root canal of upper molar tooth
- Dental pulp of upper molar tooth
- Dental pulp of upper premolar tooth
- Enamel of canines tooth
- Enamel of lower molar tooth
- Mandibular nerve
- Submandibular lymph nodes
- Root canal of upper premolar tooth
- Root canal of upper canines tooth
- Enamel of upper molar tooth
- Enamel of upper incisor tooth
- Enamel of lower canines tooth
- Enamel of lower incisor tooth
- Enamel of lower premolar tooth
- Dental pulp of lower molar tooth
- Root canal of lower canines tooth
- Alveolar ridge
- Root canal of lower premolar tooth
- Lower premolar apical foramen
- Dental branches of inferior alveolar artery, vein, & nerve
- Alveolar process of maxilla
- Superior dental plexus
- Root of lower canines tooth
- Body of tongue
- Dorsum of tongue
- Malar (zygomatic) lymph nodes
- Preauricular lymph nodes
- Nasolabial lymph nodes
- Superficial parotid lymph nodes
- Buccinator lymph nodes
- Deep parotid lymph nodes
- Retropharyngeal lymph nodes
- Mastoid lymph nodes
- Occipital lymph nodes
- Superior deep cervical lymph nodes
- Mandibular lymph nodes
- Lingual lymph nodes
- Jugulodigastric lymph nodes
- Accessory lymph nodes
- Submental lymph nodes
- Superficial lateral cervical lymph nodes
- Middle deep cervical lymph nodes
- Superficial anterior cervical lymph nodes
- Thyroid lymph nodes
- Paratracheal lymph nodes
- Inferior deep cervical lymph nodes
- Supraclavicular lymph nodes
- Axis (C2 vertebra)
- C3–C4 intervertebral disc
- Anulus fibrosus of intervertebral disc
- Nucleus pulposus of intervertebral disc
- Lamina of vertebra
- Spinous process of vertebra
- Facet joint of vertebra (Zygapophyseal joints)
- Atlantooccipital joint
- Anterior tubercle of atlas
- Lateral atlantoaxial joint
- Transverse process of atlas
- Anterior longitudinal ligament
- Posterior longitudinal ligament
- Ligamenta flava (Ligamentum flavum)
- Interspinous ligament
- Alar ligament
- Anterior atlantooccipital membrane
- Posterior atlantooccipital membrane
- Levator scapulae muscle
- Right vertebral artery
- Left vertebral artery
- Right vertebral artery (cervical part)
- Right vertebral artery (atlantic part)
- Right Vertebral Artery (Intracranial Part)
- Left Vertebral Artery (Intracranial Part)
- Left vertebral artery (atlantic part)
- Left vertebral artery (cervical part)
- subarachnoid space of spinal cord
- Ventral root of spinal nerve
- Dorsal root of spinal nerve
- Cisterna magna
- Body of vertebra
- Pedicle of vertebra
- Transverse process of vertebra
- Superior articular process of vertebra
- Inferior articular process of vertebra
- Intervertebral Disc
- Rotatores cervicis muscles
- Oblique and transverse arytenoid muscles
- Inferior constrictor muscle of pharynx
- Pharyngeal raphe
- Exit foramina
- Transverse foramen
- Premedullary cistern
- Median aperture of fourth ventricle (foramen of Magendie)
- Median sulcus of rhomboid fossa
- Cerebellopontine cistern
- Lateral aperture of fourth ventricle (foramen of Luschka)
- Sylvian cistern
- Cerebral aqueduct
- Choroid fissure
- Superior opening of cerebral aqueduct
- Collateral trigone
- Transverse pontine vein
- Inferior cerebellar veins
- Lateral occipital artery
- Flocculus
- Crus I of ansiform lobule of cerebellum
- Crus II of ansiform lobule of cerebellum
- Paramedian lobule (HVII) of cerebellum
- Simple lobule (HVI) of cerebellum
- Anterior quadrangular lobule (HV) of cerebellum
- Anterior quadrangular lobule (HlV) of cerebellum
- Biventral lobule (HVIII) of cerebellum
- White matter of cerebellum (Arbor vitae)
- Intrabiventral Fissure of Biventral Lobule
- Lunogranicile fissure of cerebellum
- Medial occipital artery
- Posterior inferior cerebellar artery
- Lingula of cerebellum (I)
- Central lobule (II & III) of Cerebellum
- Culmen (IV, V) of Cerebellum
- Declive (VI) of Cerebellum
- Folium (VII) of Cerebellum
- Tuber of vermis (VII)
- Pyramid of vermis (VIII)
- Uvula of vermis (IX)
- Nodule of vermis (X)
- Cerebellar tonsil (H IX)
- Pineal gland
- Calcarine artery
- Parieto-occipital artery
- Posterior hippocampal artery
- Anterior parietal artery
- Rolandiс artery
- Pre-Rolandic artery
- Frontopolar artery
- Temporopolar artery
- Lateral orbitofrontal artery
- Medial orbitofrontal artery
- Middle meningeal artery
- Anterior cerebral artery (A1 Segment)
- Anterior cerebral artery (A2 Segment)
- Anterior cerebral artery (A3 Segment)
- Posterior cerebral artery (P1 Segment)
- Posterior cerebral artery (P2 Segment)
- Posterior cerebral artery (P3 Segment)
- Posterior cerebral artery (P4 Segment)
- Middle cerebral artery horizontal segment (M1)
- Middle cerebral artery insular segment (M2)
- Middle cerebral artery opercular segment (M3)
- Middle cerebral artery cortical segment (M4)
- Superior cortical veins
- Deep middle cerebral vein
- Posterior vein of septum pellucidum
- Vein of cerebellomedullary cistern
- Inferior vermian vein
- Superior vermian vein
- Inferior choroidal vein
- Angular vein
- Supratrochlear veins
- Common facial vein
- Lingual vein
- Posterior external vertebral venous plexus
- Anterior internal vertebral venous plexus
- Anterior external vertebral venous plexuses
- Body of hippocampus
- Head of hippocampus
- Tail of hippocampus
- Hippocampus
- Anterior hippocampal veins
- Choroid plexus
- Thoracic part of esophagus
- Trachea
- Right lobe of thyroid gland
- Left lobe of thyroid gland
- Thyroid gland
- Left lobe of liver
- Right lobe of liver
- Liver
- Manubrium of sternum
- Body of sternum
- Xiphoid process of sternum
- Sternum
- Pericardium
- Heart
- Left ventricle
- Right atrium
- Left atrium
- Right ventricle
- Left auricle
- Coronary sinus
- Pulmonary trunk
- Pulmonary valve
- Conus arteriosus
- Interventricular Septum
- Left atrioventricular valve (mitral or bicuspid valve)
- Right atrioventricular valve (tricuspid valve)
- Aortic sinus
- Aortic root
- Ascending aorta
- Arch of aorta
- Descending thoracic aorta
- Thymus
- Thymic veins
- Spleen
- Gallbladder
- Pancreas
- Fundus of stomach
- Body of stomach
- Cardia of stomach
- Pylorus of stomach
- Pyloric canal
- pyloric antrum
- Transverse colon
- Descending colon
- Esophagus
- Costal cartilages
- Costal notches
- Costochondral joints
- Costovertebral joint
- Costoxiphoid ligaments
- Sternocostal joint
- Sternocostal synchondrosis of first rib
- Pleura
- Sternal part of diaphragm
- Costal part of diaphragm
- Lumbar part of diaphragm
- Left hemidiaphragm
- Right hemidiaphragm
- Diaphragm
- Crura of diaphragm
- Right crus of diaphragm
- Median arcuate ligament
- Axillary lymph nodes
- Infraclavicular lymph nodes
- Right main bronchus
- Left main bronchus
- Right apical segmental bronchus (B1)
- Left apicoposterior bronchus (B1+2a, B1+2b)
- Right posterior segmental bronchus (B2, B2a, B2b)
- Right anterior segmental bronchus (B3)
- Left anterior segmental bronchus (B3a, B3b, B3c)
- Superior lingular bronchus of left lung (B4)
- Inferior lingular bronchus of left lung (B5)
- Left inferior lobar bronchus
- Right middle lobe bronchus
- Right lung (superior lobe)
- Right lung (middle lobe)
- Right lung (inferior lobe)
- Left Lung (Superior Lobe)
- Left lung (inferior lobe)
- Oblique fissure of left lung
- Oblique fissure of right lung
- Horizontal fissure of right lung
- Lingular bronchus of left lung
- Left superior lobar bronchus
- Anteromedial basal bronchus of left lung (B7+8)
- Posterior basal segmental bronchus of left lung (B10)
- Lateral basal segmental bronchus of left lung (B9)
- Posterior basal segmental bronchus of right lung (B10)
- Lateral basal segmental bronchus of right lung (B9)
- Anterior basal segmental bronchus of right lung (B7+8, B8)
- Medial segmental bronchus of right lung (B5)
- Superior segmental bronchus of right lung (B6)
- Right intermediate bronchus
- Right adrenal gland
- Left adrenal gland
- Adrenal glands
- Posterior sternoclavicular ligament
- Superior sternopericardial ligaments
- Sternal end of the clavicle
- Thoracoacromial artery
- Subscapular artery
- Thoracodorsal artery
- Lateral thoracic artery
- Circumflex scapular artery
- Dorsal scapular artery
- Suprascapular artery
- Superior intercostal artery
- Thyrocervical trunk
- Axillary artery
- Left common carotid artery
- Internal thoracic artery
- Superior phrenic artery
- Posterior intercostal arteries
- Right hepatic artery
- Left hepatic artery
- Left gastric artery
- Proper hepatic artery
- Gastroduodenal artery
- Common hepatic artery
- Splenic artery
- Celiac trunk
- Abdominal aorta
- left gastro-omental artery (left gastroepiploic artery)
- Short gastric arteries
- Left anterior descending artery (LAD)
- Circumflex artery (LCx)
- Left main coronary artery (LMCA)
- Right coronary artery (RCA)
- First diagonal branch (D1) of LAD
- Second diagonal branch (D2) of LAD
- Third diagonal branch (D3) of LAD
- Sinoatrial nodal artery
- Conus artery
- Acute marginal artery (AM)
- Interventricular septal branch S1
- Interventricular septal branch S2
- Left marginal vein
- First obtuse marginal branch
- Anterior interventricular sulcus
- Small cardiac vein
- Great cardiac vein
- Middle cardiac vein
- Posterior vein of left ventricle
- Right marginal vein of heart
- Valve of coronary sinus
- Inferior vena cava
- Azygos vein
- Anterior leaflet of left atrioventricular valve
- Posterior leaflet of left atrioventricular valve
- Pectinate muscles
- Sulcus terminalis of heart
- Trabeculae carneae
- Anterior papillary muscle
- Posterior papillary muscle
- Myocardium
- Endocardium
- Epicardium
- Coronary sulcus
- Posterior interventricular sulcus
- Pericardial cavity
- Thoracic duct
- Sinoatrial node (SA node)
- Atrioventricular Node (AV Node)
- Atrioventricular bundle (bundle of His)
- Right branch of atrioventricular bundle
- Left branch of atrioventricular bundle
- Oblique vein of left atrium
- Left atrial branch (coronary artery)
- Openings of pulmonary veins
- Oval fossa of right atrium
- Right fibrous trigone
- Right auricle of heart
- Aortic vestibule
- Interatrial septum
- Noncoronary aortic sinus
- Aortic valve
- Superior vena cava
- Opening of superior vena cava
- Opening of inferior vena cava
- Sinus of venae cavae (sinus venarum)
- Hemiazygos vein
- Superior tracheobronchial lymph nodes
- Subcarinal lymph nodes
- Interlobar lymph nodes
- Inferior tracheobronchial lymph nodes
- Transverse pericardial sinus
- Oblique pericardial sinus
- Middle lobar artery of right lung
- Inferior lobar artery of right lung
- Lateral segmental artery of right Lung
- Anterior basal segmental artery of right lung
- Lateral basal segmental artery of right lung
- Posterior basal segmental artery of right lung
- Anterior basal segmental artery of left lung
- Posterior basal segmental artery of left lung
- Lateral basal segmental artery of left lung
- Right superior pulmonary vein
- Right inferior pulmonary vein
- Left superior pulmonary vein
- Left inferior pulmonary vein
- Right middle lobe vein
- Superior vein of right lung
- Medial vein of right lung
- Lateral vein of right lung
- Common basal vein of right lung
- Posterior basal vein of right lung
- Lateral basal vein of right lung
- Superior vein of left lung
- Posterior basal vein of left lung
- Lingular vein of left lung
- Anterior basal vein of left lung
- Crista terminalis
- Carina of trachea
- Right superior lobar bronchus
- Right middle lobar bronchus
- Right inferior lobar bronchus
- Anterior segmental bronchus of right lung
- Apical segmental bronchus of right lung
- Apicoposterior segmental bronchus of left lung
- Superior lobar artery of right lung
- Superior lobar artery left lung
- Brachial artery
- Left pulmonary artery
- Right pulmonary artery
- Anterior segmental artery of left lung
- Anterior segmental artery of right lung
- Apical segmental artery of right lung
- Apical segmental artery of left lung
- Posterior segmental artery of left lung
- Posterior segmental artery right lung
- Superior segmental artery of left lung
- Superior segmental artery of right lung
- Superior lingular artery of left lung
- Medial segmental artery of right lung
- Inferior phrenic artery
- Splenic branches of splenic artery
- Right interlobar artery
- Left interlobar artery
- Subsuperior segmental artery of right lung
- Jugular venous arch
- Inferior thyroid vein
- Vertebral vein
- Left brachiocephalic vein
- Left subclavian vein
- Right subclavian vein
- Axillary veins
- Brachial veins
- Thoracodorsal vein
- Dorsal scapular vein
- Suprascapular vein
- Right brachiocephalic vein
- Intermediate hepatic vein
- Right hepatic vein
- Left hepatic vein
- Left gastro-omental (gastroepiploic) vein
- Short gastric veins
- Hepatic portal vein
- Splenic vein
- Inferior phrenic vein
- Anterior vein of left lung
- Anterior vein of right lung
- Posterior vein of right lung
- Superior lingular vein of left lung
- Inferior lingular vein of left lung
- Tracheal bifurcation
- Posterior segmental bronchus of right lung
- Lateral segmental bronchus of right lung
- Glenoid fossa
- Glenoid process of scapula
- Spine of scapula
- Acromion process of scapula
- Coracoid process of scapula
- Scapular body
- supraspinous fossa of scapula
- Subscapular fossa
- Neck of scapula
- Humerus
- Head of humerus
- Body of humerus
- Shaft (body) of clavicle
- Acromial end of clavicle
- Sternoclavicular joint
- Costovertebral joint of first rib (rib head joint)
- Costotransverse joint of first rib
- Tubercle of rib
- Ribs
- Intra-articular ligament of head of rib
- Pectoralis minor muscle
- Latissimus dorsi muscle
- Coracobrachialis muscle
- Teres major muscle
- Subscapularis muscle
- Teres minor muscle
- Infraspinatus muscle
- Rotatores muscle
- Semispinalis muscle
- Spinalis muscle
- Iliocostalis muscle
- Longissimus muscle
- Levatores costarum muscle
- Rectus abdominis muscle
- External oblique muscle
- Serratus posterior inferior muscle
- Brachial plexus
- Spinal nerves
- Left recurrent laryngeal nerve
- Left phrenic nerve
- Intervertebral foramina
- Intertransverse ligament
- Costotransverse ligament
- Basivertebral veins
- Anterior cecal artery
- Appendicular artery
- Cystic artery
- Ileal arteries
- Ileocolic artery
- Ileocolic artery colic branches
- Ileocolic artery ileal branches
- Inferior mesenteric artery (IMA)
- Interlobar arteries of kidney
- Jejunal arteries
- Left colic artery
- Marginal artery of Drummond
- Middle colic artery
- Omental branches of gastro-omental (gastroepiploic) artery
- Right posterior descending coronary artery (Right PDA)
- Distal left anterior descending artery (dLAD)
- Right colic artery
- Right gastric artery
- Superior epigastric artery
- Superior mesenteric artery (SMA)
- Superior rectal artery
- Accessory hepatic vein
- Great pancreatic vein
- Left branch of hepatic portal vein
- Right branch of hepatic portal vein
- Portal vein branch to liver segment I
- Portal vein branch to liver segment II
- Portal vein branch to liver segment III
- Portal vein branch to liver segment IV
- Portal vein branch to liver segment V
- Portal vein branch to liver segment VI
- Portal vein branch to liver segment VII
- Portal vein branch to liver segment VIII
- Right gastric vein
- Internal thoracic veins
- Left internal thoracic veins
- Right internal thoracic veins
- Right internal thoracic artery
- Left internal thoracic artery
- Right ovarian vein
- Left ovarian vein
- Superior epigastric veins
- Sigmoid veins
- Vasa recta (kidney)
- Superior mesenteric vein
- Superior rectal vein
- Posterior intercostal veins
- Abdominal part of esophagus
- Ascending colon
- Cardia of stomach
- Cecum
- Duodenum – Superior part (D1)
- Duodenum – Descending part (D2)
- Duodenum – Horizontal part (D3)
- Duodenum – Ascending part (D4)
- Fundus of gallbladder
- Body of gallbladder
- Neck of gallbladder
- Ileocaecal valve (ileocecal junction)
- Jejunum
- Ileum
- Terminal ileum
- Small intestine
- Stomach
- Transverse mesocolon
- Descending mesocolon
- Ascending mesocolon
- Right paracolic gutter
- Left paracolic gutter
- kidneys
- Right kidney
- Left kidney
- Kidney cortex (Renal cortex)
- Renal capsule
- Renal medulla
- Renal pyramids
- Adrenal gland
- Ureters
- Left ureter
- Right ureter
- Ureteropelvic junction
- Renal fascia
- Renal artery
- Renal vein
- Left renal vein
- Right renal vein
- Paraesophageal lymph nodes
- Prepericardial lymph nodes
- Superior diaphragmatic lymph nodes
- Superior mesenteric lymph nodes
- Lateral aortic lymph nodes
- Lesser curvature lymph nodes
- Apex of the heart
- Phrenicomediastinal recess
- Crural part of diaphragm
- Phrenoesophageal ligament
- Internal oblique muscle
- Transversus abdominis muscle
- Iliacus muscle
- Psoas major muscle
- Quadratus lumborum muscle
- Intercostal muscles
- Interspinales muscles
- Intertransversarii muscle
- Gluteus maximus muscle
- Gluteus medius muscle
- Gluteus minimus muscle
- Transversus thoracis muscle
- Cauda equina
- Conus medullaris
- Aortic bifurcation
- Ala of ilium (wing of ilium)
- Iliac crest
- Iliac tubercle
- Sacrum
- Ala of sacrum
- Coccyx
- Median sacral crest
- Sacral canal
- Posterior sacral foramina
- Anterior sacral foramina
- Posterior superior iliac spine
- Posterior inferior iliac spine
- Transverse processes
- Sacroiliac joint
- Supraspinous ligament
- Falciform ligament (liver)
- Ligamentum teres (round ligament of the liver)
- Umbilical vein
- Ligamentum venosum
- Fissure for ligamentum venosum
- Fissure for ligamentum teres
- Linea alba
- Lumbar triangle
- Parietal peritoneum
- Preperitoneal space
- Quadrate lobe of liver
- Caudate lobe of liver
- Liver Segment I – Caudate lobe
- Liver Segment II – Left lateral superior segment
- Liver Segment III – Left lateral inferior segment
- Liver Segment IVa – Left medial superior segment
- Liver Segment IVb – Left medial inferior segment
- Liver Segment V – Right anteroinferior segment
- Liver Segment VI – Right posteroinferior segment
- Liver Segment VII – Right posterosuperior segment
- Liver Segment VIII – Right anterosuperior segment
- Acetabular margin (Acetabular rim)
- Acetabulum
- Anterior acetabular wall
- Posterior acetabular wall
- Anterior superior iliac spine
- Anterior inferior iliac spine
- Body of femur
- Body of ilium
- Body of ischium
- Body of pubis
- Ilium bone
- Ischium bone
- Pubic bone
- Greater sciatic notch
- Greater trochanter
- Lesser trochanter
- Head of femur
- Neck of femur
- Iliopubic eminence
- Inferior pubic ramus
- Intertrochanteric line
- Ischial spine
- Ischial tuberosity
- Ramus of ischium
- Superior pubic ramus
- Pudendal nerve
- Sciatic nerve
- Obturator nerve
- Accessory obturator artery
- Deep circumflex iliac artery
- Inferior gluteal artery
- Lateral circumflex femoral artery
- Deep femoral artery (profunda femoris)
- External iliac artery
- Femoral artery
- Internal iliac artery
- Medial circumflex femoral artery
- Obturator artery
- Superficial femoral artery
- Pudendal artery
- Superficial circumflex iliac artery
- Umbilical artery
- Uterine artery
- Superior gluteal artery
- Accessory obturator vein
- Accessory saphenous vein
- Inferior gluteal vein
- Lateral circumflex femoral veins
- External iliac vein
- Femoral vein
- great saphenous vein
- Internal iliac vein
- Medial circumflex femoral vein
- Obturator vein
- Pudendal vein
- Superficial circumflex iliac vein
- Uterine venous plexus
- Vaginal venous plexus
- Common iliac vein
- Union of common iliac veins
- common iliac artery
- Adductor brevis muscle
- Adductor longus muscle
- Adductor magnus muscle
- Adductor minimus muscle
- Coccygeus muscle
- External anal sphincter
- Internal anal sphincter
- Gracilis muscle
- Inferior gemellus muscle
- Superior gemellus muscle
- Levator ani muscle
- Obturator externus muscle
- Obturator internus muscle
- Pectineus muscle
- Puborectalis muscle
- Pyramidal muscle (pyramidalis muscle)
- Rectus femoris muscle
- Sartorius muscle
- Tensor fasciae latae muscle
- Vastus lateralis muscle
- Vastus medialis muscle
- Anal canal
- Anococcygeal body (anococcygeal ligament)
- Iliofemoral ligament
- Iliotibial tract
- Female urethra
- Inferior pubic ligament
- Superior pubic ligament
- Inguinal ligament
- Inguinal lymph nodes
- Internal urethral orifice
- Intermediate lacunar external iliac lymph nodes
- Ischioanal fossa
- External iliac lymph nodes
- Median umbilical ligament
- Mesorectal fascia
- Uterosacral ligament
- Mesorectum
- Obturator lymph nodes
- Pubic symphysis
- Rectovaginal septum (rectovaginal fascia)
- Rectum
- Sacrospinous ligament
- Sacrotuberous ligament
- Vesicovaginal space
- Urinary bladder
- Iliopsoas tendon
- Uterus
- Body of uterus
- Fundus of uterus
- Cervix of uterus
- Isthmus of uterus
- Vagina
- Fornix of the vagina
- Endometrium of uterus
- Myometrium of uterus
- Perimetrium of uterus
- Junctional zone of uterus
- Ovaries
- Right ovary
- Left ovary
- Fallopian tube
- Suspensory ligament of ovary
- Broad ligament of uterus
- Round ligament of uterus
- Piriformis muscle
- Saphenous nerve
- Muscular branches of femoral nerve
- Lateral femoral cutaneous nerve
- Obturator veins
- Posterior division of obturator nerve (Posterior branch of obturator nerve)
- Anterior division of obturator nerve (Anterior branch of obturator nerve)
- Coccygeal nerve
- Coccygeal plexus
- Uterine horn
- Endocervical canal
- Stroma of the cervix
- Internal os of the cervix
- External os of the cervix
- Vesicouterine pouch
- Rectouterine pouch (pouch of Douglas)
- Mons pubis
- Pubic tubercle
- Retropubic space
- Urethrovaginal space
- External urethral sphincter (female)
- Internal urethral sphincter (female)
- Internal urethral sphincter (male)
- External urethral sphincter (male)
- Superficial transverse perineal muscle
- Deep transverse perineal muscle
- Ischiocavernosus muscle (Female)
- Bulbospongiosus muscle (Female)
- Bulbospongiosus muscle (Male)
- Ischiocavernosus muscle (Male)
- Labia majora
- Labia minora
- Clitoris
- Skene’s gland (paraurethral glands)
- Vestibular fossa
- External urethral orifice
- Rectococcygeal muscle
- Vas deferens
- Inferior epigastric artery
- Inferior epigastric veins
- Superior vesical artery
- Inferior vesical artery
- Testicular artery
- Vesical veins
- Vesical venous plexus
- Posterior femoral cutaneous nerve
- Gluteal lymph nodes
- Sacral lymph nodes
- Puboprostatic ligament
- Trigone of urinary bladder
- Apex of urinary bladder
- Neck of urinary bladder
- Fundus of urinary bladder
- Body of urinary bladder
- Seminal vesicle
- Ejaculatory duct
- Peripheral zone of prostate
- Anterior Fibromuscular Stroma of prostate
- Central zone of prostate
- Transitional zone of prostate
- Obturator internus tendon
- Obturator externus tendon
- Puboprostaticus muscle
- Puboanalis muscle
- Pubococcygeus muscle
- Iliococcygeus muscle
- Ischiococcygeus muscle
- Membranous urethra
- Prostatic urethra
- Penile urethra
- Rectoprostatic fascia (Denonvilliers' fascia)
- Rectosacral fascia (Waldeyer's fascia)
- Presacral fascia
- Fascia of pelvic diaphragm
- Rectal proper fascia (Fascia propria of the rectum)
- Genitofemoral nerve
- Femoral nerve
- Anterior lateral femoral cutaneous nerve
- Posterior lateral femoral cutaneous nerve
- Intercommunicating branches of L3–L4 nerves
- Traversing nerve root of spinal nerve
- Exiting nerve root of spinal nerve
- Spinal nerve L1
- Spinal nerve L2
- Spinal nerve L3
- Spinal nerve L4
- Spinal nerve L5
- Spinal nerve S1
- Spinal nerve S2
- Spinal nerve S3
- Spinal nerve S4
- Iliohypogastric nerve
- Ilioinguinal nerve
- Superior cluneal nerves
- Medial cluneal nerves
- Superior gluteal nerve
- Lumbosacral trunk
- Sacral plexus
- Inferior rectal nerve
- Perineal nerves
- Dorsal ramus of spinal nerve
- Inferior gluteal nerve
- Sacral splanchnic nerves
- Anococcygeal nerve
- Spermatic cord
- Cremaster muscle
- Bulbourethral gland (Cowper’s glands)
- Rectovesical pouch
- Spermatic cord nerves
- Pampiniform plexus
- Transverse perineal muscle
- Buck's fascia (Deep fascia of penis)
- Dartos fascia
- Areolar tissue of penis
- Subcutaneous tissue (scrotum)
- Septum of the penis (Penile septum)
- Corpus cavernosum
- Corpus spongiosum
- Bulb of Penis
- Crus of penis
- Head of epididymis
- Tail of epididymis
- Body of epididymis
- Epididymis
- Deep dorsal vein of the penis
- Superficial dorsal vein of penis
- Foreskin
- Glans penis
- Corona of glans penis
- Coronal sulcus
- Meatus of the urethra
- Testis
- Tunica albuginea (penis)
- Tunica albuginea of testis
- Septum of scrotum
- Skin of scrotum
- External spermatic fascia
- Cremaster fascia
- Internal spermatic fascia
- Parietal tunica vaginalis
- Lobule of testis
- Mediastinum testis
- Visceral tunica vaginalis
- Scrotal fluid
- Septum of testis
- Anterior sacroiliac ligament
- Interosseous sacroiliac ligament
- Posterior sacroiliac ligament
- Uterine veins
- Sigmoid colon
- Sacral venous plexus
- Superior gluteal veins
- Lateral sacral artery
- Lateral sacral vein
- Median sacral vein
- Internal iliac lymph nodes
- Lateral part of sacrum
- Transverse ridges
- Sacral cornu (sacral horn)
- Sacral hiatus
- Intermediate sacral crest
- Mesorectal free fluid
- Lumbar arteries
- Common iliac lymph nodes
- Spinal nerve S5
- Spinal nerve Co1
- Iliolumbar ligament
- Lumbosacral joint
- Superior articular process of S1 vertebra
- Inferior articular process of L5 vertebra
- Lateral sacral crest
- Exiting nerve root of spinal nerve S1
- Traversing nerve root of spinal nerve S1
- Traversing nerve root of spinal nerve S2
- Traversing nerve root of spinal nerve S3
- Traversing nerve root of spinal nerve S4
- Exiting nerve root of spinal nerve S2
- Exiting nerve root of spinal nerve S3
- Exiting nerve root of spinal nerve S4
- Exiting nerve root of spinal nerve S5
- Filum terminale internum
- Lumbar veins
- Renal pelvis
- Vertebral venous plexus
- Common bile duct
- Left crus of diaphragm
- Right lumbar part of diaphragm
- Left lumbar part of diaphragm
- Thoracolumbar fascia (posterior layer)
- Thoracolumbar fascia (middle layer)
- Thoracolumbar fascia (anterior layer)
- Costovertebral joint of twelfth rib
- Costotransverse joint of twelfth rib
- Head of twelfth rib
- Mammillary process of vertebra
- Accessory process of vertebrae
- Spinal dura mater
- Spinal epidural space
- Dorsal traversing nerve root
- Ventral traversing nerve root
- Dorsal exiting nerve root
- Ventral exiting nerve root
- Dorsal root ganglion of spinal nerve
- Iliocostalis lumborum muscle
- Longissimus thoracis muscle
- Spinalis thoracis muscle
- Rotatores thoracis muscles
- Rotatores lumborum muscles
- Lateral intertransversarii lumborum muscle
- Medial intertransversarii lumborum
- Interspinales lumborum muscle
- Annulus fibrosus of intervertebral disc
- Iliac tuberosity
- Inferior mesenteric vein
- L5–S1 Intervertebral disc
- L4–L5 Intervertebral Disc
- L3–L4 Intervertebral Disc
- L2–L3 Intervertebral Disc
- L1–L2 Intervertebral Disc
- T12–L1 Intervertebral Disc
- Vertebrae
- Thoracic aorta
- Duodenal bulb
- Right colic flexure (hepatic flexure)
- Left colic flexure (splenic flexure)
- Common hepatic duct
- Left hepatic duct
- Right hepatic duct
- Lateral branch of left hepatic duct
- Anterior branch of right hepatic duct
- Posterior branch of right hepatic duct
- Cystic duct
- Pancreatic duct
- Left renal artery
- Right renal artery
- Neck of pancreas
- Head of pancreas
- Uncinate process of pancreas
- Body of pancreas
- Tail of pancreas
- Accessory pancreatic duct
- Hepatopancreatic ampulla (ampulla of Vater)
- Bile duct serving liver segment I
- Bile duct serving liver segment II
- Bile duct serving liver segment III
- Bile duct serving liver segment IVa
- Bile duct serving liver segment IVb
- Bile duct serving liver segment V
- Bile duct serving liver segment VI
- Bile duct serving liver segment VII
- Bile duct serving liver segment VIII
- Placenta
- Uterus (pregnancy)
- Amniotic fluid
- Umbilical cord
- Urinary Bladder in Pregnancy
- Cervix in Pregnancy
- Vagina in Pregnancy
- Fundus of uterus in pregnancy
- Fetal brain
- Fetal caudate nucleus
- Fetal thalamus
- Fetal pons
- Fetal cerebellum
- Fetal occipital lobe
- Fetal temporal lobe
- Fetal parietal lobe
- Fetal frontal lobe
- Fetal third ventricle
- Fetal fourth ventricle
- Fetal lateral ventricle
- Fetal superior sagittal sinus
- Fetal straight sinus
- Fetal transverse sinus
- Fetal sigmoid sinus
- Fetal cervical spine
- Fetal thoracic spine
- Fetal lumbar spine
- Fetal spinal cord
- Fetal Eyes
- Fetal paranasal sinuses
- Fetal tooth buds
- Maternal ovaries
- Fetal shoulder
- Fetal lungs
- Fetal Ribs
- Fetal trachea
- Fetal Heart
- Fetal aorta
- Fetal upper arm
- Fetal knee
- Fetal ankle
- Fetal foot
- Fetal thigh
- Fetal Lower Leg
- Fetal forearm
- Fetal Liver
- Fetal small bowel
- Fetal hand
- Fetal urinary bladder
- Fetal kidneys
- Fetal rectum
- Fetal elbow
- Fetal wrist
- Fetal hip
- Fetal anus
- Fetal Fingers
- Fetal buttock
- Fetal scrotum
- Fetal testis
- Fetal penis
- Fetal colon
- Fetal stomach
- Fetal spinal canal
- Iliopsoas muscle
- Vastus intermedius muscle
- Quadratus femoris muscle
- Erector spinae muscles
- Rectus femoris tendon (Proximal tendon of rectus femoris)
- Sartorius Tendon (Proximal)
- Gluteus minimus tendon
- Gluteus medius tendon
- Tensor fasciae latae tendon
- Conjoint tendon of biceps femoris & semitendinosus
- Semimembranosus tendon (proximal)
- Deep femoral vein (profunda femoris vein)
- Femoral shaft
- Femur
- Ischiopubic ramus
- Superficial inguinal lymph nodes
- Pubofemoral ligament
- Zona orbicularis ligament
- Ligamentum teres (ligament of the head of femur)
- Acetabular labrum
- Ischiofemoral ligament
- Transverse acetabular ligament
- Iliofemoral Ligament superior band (transverse band, lateral band)
- Iliofemoral Ligament inferior band (vertical band, medial band)
- Articular capsule of hip joint
- Biceps femoris muscle (Short head)
- Biceps femoris muscle (Long head)
- Semitendinosus muscle
- Semimembranosus muscle
- Gracilis Tendon (Proximal)
- Plantaris muscle
- Lateral head of gastrocnemius muscle
- Medial head of gastrocnemius muscle
- Gastrocnemius muscle
- Popliteus muscle
- Soleus muscle
- Vastus Lateralis Obliquus Muscle
- Extensor digitorum longus muscle
- Tibialis anterior muscle
- Fibularis longus muscle (peroneus longus muscle)
- Patellar tendon (patellar ligament)
- Medial gastrocnemius tendon
- Lateral gastrocnemius tendon
- Distal biceps femoris tendon
- Distal semimembranosus tendon
- Distal semitendinosus tendon
- Gracilis tendon (Distal)
- Sartorius tendon (Distal)
- Distal quadriceps femoris tendon
- Distal vastus intermedius tendon
- Distal rectus femoris tendon
- Distal vastus medialis tendon
- Distal vastus lateralis tendon
- Popliteus tendon
- Distal adductor magnus tendon
- Medial collateral ligament
- Lateral collateral ligament
- Anterior cruciate ligament
- Posterior cruciate ligament
- Anterolateral ligament of knee
- Posterior meniscofemoral ligament
- Anterior meniscofemoral ligament
- Oblique popliteal ligament
- Arcuate popliteal ligament
- Medial patellofemoral ligament
- Lateral patellofemoral ligament
- Medial patellar retinaculum
- Lateral patellar retinaculum
- Transverse ligament of knee
- Anterior ligament of fibular head
- Posterior ligament of fibular head
- Popliteal artery
- Descending genicular artery (Saphenous branch)
- Descending genicular artery (Articular branches)
- Superior medial genicular artery
- Superior lateral genicular artery
- Perforating Arteries (Knee joint)
- Popliteal vein
- Inferior lateral genicular artery
- Small saphenous vein
- Superior lateral genicular vein
- Superior medial genicular vein
- Inferior lateral genicular vein
- Popliteal–Saphenous perforating veins
- Medial epicondyle of femur
- Lateral epicondyle of femur
- Lateral condyle of femur
- Medial condyle of femur
- Femoral condyle articular cartilage
- Tibial condyle articular cartilage
- Body of tibia
- Tibial tuberosity
- Lateral intercondylar tubercle
- Medial intercondylar tubercle
- Tibia
- Fibula
- Head of fibula
- Neck of fibula
- Medial tibial plateau
- Lateral tibial plateau
- Base of patella
- Apex of patella
- Medial border of patella
- Lateral border of patella
- Medial articular facet of patella
- Lateral articular facet of patella
- Patella
- Patellar articular cartilage
- Infrapatellar fat pad
- Suprapatellar fat pad
- Prefemoral fat pad
- Popliteal lymph nodes
- Trochlear groove
- Common fibular nerve
- Tibial nerve
- Muscular branches of tibial nerve
- Infrapatellar branch of saphenous nerve
- Lateral sural cutaneous nerve
- Medial sural cutaneous nerve
- Gerdy’s tubercle
- Meniscus cartilage
- Medial meniscus
- Lateral meniscus
- Anterior horn of medial meniscus
- Posterior horn of medial meniscus
- Body of medial meniscus
- Anterior root of medial meniscus
- Posterior root of medial meniscus
- Anterior horn of lateral meniscus
- Posterior horn of lateral meniscus
- Body of lateral meniscus
- Anterior root of lateral meniscus
- Posterior root of lateral meniscus
- Tibiofibular joint (proximal)
- Knee Joint
- Hip joint
- Talus
- Head of talus
- Body of talus
- Neck of talus
- Posterior talar articular facet
- Calcaneus
- Anterior process of calcaneus
- Sustentaculum tali
- Tuberosity of navicular bone
- Cuboid
- Calcaneal process of cuboid bone
- Fibula shaft
- Medial malleolus
- Lateral malleolus
- Ankle joint
- Talocalcaneal joint
- Talocalcaneonavicular joint
- Calcaneocuboid joint
- Cuneocuboid Joint
- Lateral cuneiform bone
- Medial cuneiform bone
- Intermediate cuneiform bone
- Extensor hallucis longus muscle
- Fibularis tertius muscle
- Fibularis brevis muscle
- Tibialis posterior muscle
- Flexor digitorum longus muscle
- Flexor hallucis longus muscle
- Quadratus plantae muscle
- Abductor hallucis muscle
- Extensor hallucis brevis muscle
- Extensor digitorum brevis muscle
- Flexor digitorum brevis muscle
- Abductor digiti minimi muscle
- Tibialis anterior tendon
- Extensor hallucis longus tendon
- Extensor digitorum longus tendon
- Fibularis tertius tendon
- Fibularis brevis tendon
- Fibularis longus tendon
- Tibialis posterior tendon
- Tibialis posterior tendon (medial slip)
- Tibialis posterior tendon (lateral slips)
- Tibialis posterior tendon (cuneiform insertions)
- Tibialis posterior tendon (metatarsal insertions)
- Flexor digitorum longus tendon
- Flexor hallucis longus tendon
- Plantaris tendon
- Achilles tendon
- Abductor hallucis tendon
- Quadratus plantae tendon
- Anterior talofibular ligament
- Posterior talofibular ligament
- Anterior inferior tibiofibular ligament
- Accessory anterior inferior tibiofibular (Bassett’s) ligament
- Interosseous membrane (middle tibiofibular ligament)
- Posterior inferior tibiofibular ligament
- Posterior intermalleolar ligament
- Inferior transverse ligament
- Tibionavicular ligament
- Anterior tibiotalar ligament
- Tibiocalcaneal ligament
- Superficial posterior tibiotalar ligament
- Deep posterior tibiotalar ligament
- Deltoid ligament complex
- Tibiospring Ligament
- Lateral talocalcaneal ligament
- Medial talocalcaneal ligament
- Talocalcaneal interosseous ligament
- Calcaneofibular ligament
- Calcaneonavicular ligament (Bifurcate ligament)
- Calcaneocuboid ligament (Bifurcate ligament)
- Bifurcate ligament
- Spring ligament complex
- Superomedial calcaneonavicular ligament
- Medioplantar oblique calcaneonavicular ligament
- Inferoplantar longitudinal calcaneonavicular ligament
- Dorsal calcaneocuboid ligament
- Dorsal talonavicular ligament
- Superior extensor retinaculum
- Inferior extensor retinaculum
- Superior peroneal retinaculum
- Inferior peroneal retinaculum
- Flexor retinaculum
- Fascia cruris
- Kager fat pad (pre-Achilles fat pad)
- Deep fibular nerve
- Intermediate dorsal cutaneous nerve
- Medial dorsal cutaneous nerve
- Sural nerve
- Lateral dorsal cutaneous nerve
- Anastomotic branch sural nerve
- Lateral calcaneal branches of sural nerve
- Medial calcaneal nerve
- Medial calcaneal nerve (anterior cutaneous branches)
- Medial calcaneal nerve (posterior cutaneous branches)
- Inferior calcaneal nerve (Baxter’s nerve)
- Medial plantar nerve
- Lateral plantar nerve
- Posterior tibial artery
- Anterior tibial artery
- Fibular artery
- Lateral tarsal artery
- Medial tarsal arteries
- Dorsalis pedis artery
- Lateral calcaneal artery
- Medial plantar artery
- Lateral plantar artery
- Anterior tibial veins
- Posterior tibial veins
- Fibular veins
- Lateral tarsal veins
- Lateral calcaneal veins
- Medial plantar veins
- Lateral plantar veins
- Dorsal perforator veins
- Submalleolar foot perforator veins
- Calcaneal perforator veins
- Medial perforator veins of leg
- Lateral perforator veins of leg
- Plantar aponeurosis
- Dorsal cuneocuboid ligament
- Cuneocuboid interosseous ligament
- Plantar cuneocuboid ligament
- Plantar cuboideonavicular ligament
- Plantar calcaneocuboid ligament (short plantar ligament)
- Plantar cuneonavicular ligaments
- Cockett’s perforator veins
- Superficial fibular nerve
- Interosseous membrane of leg
- Dorsal cuneonavicular ligaments
- Intercuneiform ligaments
- Dorsal intercuneiform ligaments
- Plantar intercuneiform ligaments
- Interosseous intercuneiform ligaments
- Long plantar ligament
- Dorsal metatarsal ligaments
- Metatarsal interosseous ligaments
- Plantar metatarsal ligaments
- Dorsal tarsometatarsal ligaments
- Plantar tarsometatarsal ligaments
- Lisfranc ligament
- Interosseous cuneometatarsal Ligament (Lisfranc Proper Ligament)
- First dorsal cuneometatarsal ligament (Dorsal lisfranc ligament)
- First plantar cuneometatarsal ligament (Plantar lisfranc ligament)
- Cuneonavicular joint
- Cuboideonavicular joint
- Transverse tarsal joint
- Tarsometatarsal joints
- Dorsal fascia of foot
- Deep plantar arterial arch
- Dorsal venous arch of foot
- Superficial plantar venous plexus
- Navicular perforator veins
- Cuneiform perforator veins
- Navicular bone
- First metatarsal bone
- Second metatarsal bone
- Third metatarsal bone
- Fourth metatarsal bone
- Fifth metatarsal bone
- Head of metatarsal bone
- Body of the metatarsal bone
- Base of metatarsal bone
- Dorsal digital nerve of foot
- Medial branch of deep fibular nerve
- Lateral branch of deep fibular nerve
- Proper plantar digital nerve to great toe
- Flexor hallucis brevis muscle
- Lateral head of flexor hallucis brevis muscle
- Medial head of flexor hallucis brevis muscle
- Adductor hallucis muscle
- Transverse head of adductor hallucis muscle
- Oblique head of adductor hallucis muscle
- Lumbrical muscles
- Plantar interosseous muscles
- Dorsal interosseous muscles
- Flexor digiti minimi brevis muscle
- Opponens digiti minimi muscle of foot
- First dorsal interosseous muscle of foot
- Second dorsal interosseous muscle of foot
- Third dorsal interosseous muscle of foot
- Fourth dorsal interosseous muscle of foot
- First plantar interosseous muscle of foot
- Second plantar interosseous muscle of foot
- Third plantar interosseous muscle of foot
- First lumbrical muscle of foot
- Second lumbrical muscle of foot
- Third lumbrical muscle of foot
- Fourth lumbrical muscle of foot
- Extensor hallucis brevis tendon
- Extensor digitorum longus tendons
- Extensor digitorum brevis tendons
- Flexor hallucis brevis tendons
- Flexor digitorum longus tendons
- Knot of Henry
- Flexor digitorum brevis tendons
- Abductor digiti minimi tendon
- Dorsal interossei tendons of foot
- Plantar interossei tendons of foot
- Dorsal metatarsal arteries
- Plantar metatarsal arteries
- Dorsalis pedis veins
- Dorsal metatarsal veins
- Medial tarsal veins
- Medial marginal vein of foot
- Lateral marginal vein of foot
- Plantar venous arch
- Great toe (Hallux)
- Second toe
- Third toe
- Fourth toe
- Fifth toe
- Sesamoid bone of great toe
- Lateral sesamoid bone
- Medial sesamoid bone
- Proximal phalanx of foot
- Distal phalanx of foot
- Middle phalanx of foot
- Proximal phalanx of great toe
- Distal phalanx of great toe
- Base of phalanx of foot
- Head of phalanx of foot
- Body of phalanx of foot
- Body of metatarsal bone
- Dorsal digital nerves
- Proper plantar digital nerves
- Distal interphalangeal joint of foot
- Proximal interphalangeal joints of foot
- Interphalangeal joint of great toe
- Metatarsophalangeal joints
- Digital slips of plantar aponeurosis
- Lateral collateral ligament of big toe (lateral metatarsophalangeal collateral ligament)
- Medial collateral ligament of big toe (medial metatarsophalangeal collateral ligament)
- Lateral collateral ligament of interphalangeal joint of foot
- Medial collateral ligament of interphalangeal joint of foot
- Lateral sesamoid phalangeal ligament
- Medial sesamoid phalangeal ligament
- Intersesamoid ligament
- Plantar plate ligament
- Synovial fluid
- Tendon sheath
- Extensor hood of foot
- Epidermis
- Dermis of skin
- Hypodermis of skin
- Nail (toe)
- Nail bed (toe)
- Nail root (toe)
- Lateral nail fold (toe)
- Proximal nail fold
- Conoid tubercle
- Body of scapula
- Infraspinous fossa
- Anatomical neck of humerus
- Surgical neck of humerus
- Greater tubercle of humerus
- Lesser tubercle of humerus
- Shaft of humerus
- Bicipital groove
- Circumflex subscapular artery
- Posterior circumflex humeral artery
- Cephalic vein
- Posterior circumflex humeral vein
- Axillary nerve
- Ulnar nerve
- Median nerve
- Radial nerve
- Long thoracic nerve
- Dorsal scapular nerve
- Deltoid muscle
- Scapular spinal part of deltoid muscle
- Clavicular part of deltoid muscle
- Acromial part of deltoid muscle
- Biceps brachii muscle
- Short head of biceps brachii muscle
- Long head of biceps brachii muscle
- Triceps brachii muscle
- Long head of triceps brachii muscle
- Lateral head of triceps brachii muscle
- Medial head of triceps brachii muscle
- Posterior cutaneous nerve of arm
- Medial cutaneous nerve of forearm
- Long head of biceps tendon
- Short head of the biceps brachii tendon
- Deltoid Tendon (Proximal)
- Deltoid tendon (Distal)
- Teres major tendon (Distal)
- Teres minor tendon (Distal)
- Latissimus dorsi tendon
- Subscapularis tendon
- Infraspinatus tendon
- Supraspinatus tendon
- Glenohumeral ligaments
- Superior glenohumeral ligament
- Middle glenohumeral ligament
- Inferior glenohumeral ligament
- Inferior glenohumeral ligament anterior band
- Inferior glenohumeral ligament posterior band
- Inferior glenohumeral ligament, axillary pouch
- Coracohumeral ligament
- Coracoacromial ligament
- Coracoclavicular Ligaments
- Conoid ligament
- Trapezoid ligament
- Acromioclavicular ligament
- Inferior acromioclavicular ligament
- Superior acromioclavicular ligament
- Glenohumeral joint capsule
- Glenoid labrum
- Shoulder joint (glenohumeral joint)
- Acromioclavicular joint
- Articular cartilage of glenoid fossa
- Adipose tissue (Shoulder)
- Subacromial space
- Supraclavicular fossa
- Radial artery
- Ulnar artery
- Anterior ulnar recurrent artery
- Posterior ulnar recurrent artery
- Recurrent interosseous artery
- Inferior ulnar collateral artery
- Superior ulnar collateral artery
- Radial recurrent artery
- Radial collateral artery
- Middle collateral artery
- Cephalic vein of forearm
- Accessory cephalic vein
- Basilic vein
- Median cubital vein
- Accessory median cubital vein
- Median antebrachial vein
- Radial veins
- Ulnar veins
- Anterior interosseous veins
- Posterior interosseous veins
- Posterior interosseous artery
- Anterior interosseous artery
- Flexor carpi radialis muscle
- Palmaris longus muscle
- Flexor carpi ulnaris muscle
- Flexor carpi ulnaris muscle (humeral head)
- Flexor carpi ulnaris (ulnar head)
- Flexor digitorum superficialis muscle
- Flexor digitorum superficialis muscle (humeroulnar head)
- Flexor digitorum superficialis muscle (radial head)
- Flexor digitorum profundus muscle
- Pronator teres muscle
- Pronator teres muscle (humeral head)
- Pronator teres muscle (ulnar head)
- Brachialis muscle
- Brachioradialis muscle
- Extensor carpi radialis longus muscle
- Extensor carpi radialis brevis muscle
- Extensor digitorum muscle
- Extensor digiti minimi muscle
- Extensor carpi ulnaris muscle
- Extensor carpi ulnaris muscle (Humeral Head)
- Anconeus muscle
- Supinator muscle
- Articularis cubiti muscle
- Radial nerve (deep branch)
- Radial nerve (superficial branch)
- Musculocutaneous nerve
- Lateral cutaneous nerve of forearm
- Medial cutaneous nerve of forearm (anterior branch)
- Medial cutaneous nerve of forearm (posterior branch)
- Inferior lateral cutaneous nerve of arm
- Posterior cutaneous nerve of forearm
- Radius
- Ulna
- Medial epicondyle of humerus
- Lateral epicondyle of humerus
- Olecranon fossa
- Capitulum of humerus
- Trochlea of humerus
- Lateral supracondylar ridge
- Medial supracondylar ridge
- Olecranon
- Coronoid process of ulna
- Head of radius
- Neck of radius
- Body of radius
- Radial tuberosity
- Radial notch of ulna
- Trochlear notch of ulna
- Coronoid fossa
- Humeroulnar joint
- Humeroradial joint
- Proximal radioulnar joint
- Elbow joint
- Biceps brachii tendon (distal)
- Triceps brachii tendon
- Common extensor tendon
- Common flexor tendon
- Bicipital aponeurosis
- Brachial fascia
- Antebrachial fascia
- Joint capsule of elbow
- Annular ligament of radius
- Radial collateral ligament
- Lateral ulnar collateral ligament
- Lateral collateral ligament complex of elbow
- Medial collateral ligament of elbow (anterior bundle)
- Medial collateral ligament of elbow (posterior bundle)
- Medial collateral ligament of elbow (transverse bundle)
- Medial collateral ligament complex of elbow (ulnar collateral ligament)
- Quadrate ligament
- Oblique cord (ligament of Weitbrecht)
- Osborne’s ligament (cubital tunnel retinaculum)
- Cubital tunnel
- Medial intermuscular septum
- Lateral intermuscular septum
- Supratrochlear lymph nodes
- Anterior fat pad of elbow joint
- Posterior fat pad of elbow joint
- Deltoid tuberosity
- Spiral glenohumeral ligament
- Superior transverse scapular ligament
- Inferior transverse scapular ligament
- Biceps pulley
- Third metacarpal styloid process
- Dorsal radial tubercle (Lister’s tubercle)
- Radial styloid process
- Ulnar styloid process
- Body of metacarpal bone
- Head of metacarpal bone
- Base of metacarpal bone
- Carpal bones
- Metacarpal bones
- Midcarpal joint
- Radiocarpal joint (wrist joint)
- Carpometacarpal joints
- Carpal articular surface
- Scaphoid
- Lunate
- Triquetrum
- Pisiform
- Trapezium
- Trapezoid
- Tubercle of trapezium bone
- Capitate
- Hamate
- Hook of hamate bone
- Distal radioulnar joint
- First metacarpal bone (metacarpal I)
- Second metacarpal bone (metacarpal II)
- Third metacarpal bone (metacarpal III)
- Fourth metacarpal bone (metacarpal IV)
- Fifth metacarpal bone (metacarpal V)
- Head of ulna
- Tubercle of the scaphoid bone
- Abductor pollicis brevis muscle
- Flexor pollicis brevis muscle
- Flexor pollicis brevis muscle (Superficial head)
- Flexor pollicis brevis muscle (Deep head)
- Adductor pollicis muscle
- Adductor pollicis muscle (Transverse head)
- Adductor pollicis muscle (Oblique head)
- Opponens pollicis muscle
- Abductor digiti minimi muscle (hand)
- Flexor digiti minimi brevis muscle (hand)
- Opponens digiti minimi muscle (hand)
- Palmaris brevis muscle
- First dorsal interosseous muscle of hand
- Second dorsal interosseous of hand
- Third dorsal interosseous muscle of hand
- Fourth dorsal interosseous muscle of hand
- First plantar interosseous muscle of hand
- Second plantar interosseous muscle of hand
- Third plantar interosseous muscle of hand
- First lumbrical muscle of hand
- Second lumbrical muscle of hand
- Third lumbrical muscle of hand
- Fourth lumbrical muscle of hand
- Flexor pollicis longus muscle
- Pronator quadratus muscle
- Extensor pollicis longus muscle
- Extensor pollicis brevis muscle
- Abductor pollicis longus muscle
- Extensor indicis muscle
- Flexor pollicis longus tendon
- Palmaris longus tendon
- Flexor carpi radialis tendon
- Flexor carpi ulnaris tendon
- Flexor digitorum profundus tendons
- Flexor digitorum superficialis tendons
- First flexor digitorum profundus tendon
- Second flexor digitorum profundus tendon
- Third flexor digitorum profundus tendon
- Fourth flexor digitorum profundus tendon
- First flexor digitorum superficialis tendon
- Second flexor digitorum superficialis tendon
- Third flexor digitorum superficialis tendon
- Fourth flexor digitorum superficialis tendon
- Extensor carpi radialis longus tendon
- Extensor carpi radialis brevis tendon
- Extensor carpi ulnaris tendon
- Extensor digitorum tendons
- Extensor indicis tendon
- Extensor digiti minimi tendon
- Extensor pollicis longus tendon
- Extensor pollicis brevis tendon
- Abductor pollicis longus tendon
- Brachioradialis tendon
- First extensor digitorum tendon (Extensor digitorum tendon to index finger)
- Second extensor digitorum tendon (Extensor digitorum tendon to middle finger)
- Third extensor digitorum tendon (Extensor digitorum tendon to ring finger)
- Fourth extensor digitorum tendon (Extensor digitorum tendon to little finger)
- Carpal tunnel region
- Dorsal radiocarpal ligament
- Volar radioulnar ligament
- Dorsal radioulnar ligament
- Short radiolunate ligament
- Long radiolunate ligament
- Volar radioscaphocapitate ligament
- Volar scapholunate ligament
- Dorsal scapholunate ligament
- Interosseous scapholunate ligament
- Volar lunotriquetral ligament
- Dorsal lunotriquetral ligament
- Ulnotriquetral ligament
- Volar ulnolunate ligament
- Dorsal ulnolunate ligament
- Ulnocapitate ligament
- Ulnocarpal ligaments
- Pisohamate ligament
- Pisometacarpal ligament
- Ulnar collateral ligament of wrist
- Radial collateral ligament of wrist
- Dorsal intercarpal ligaments
- Capitotrapezoid ligament (Trapezocapitate ligament)
- Dorsal capitotrapezoid ligament (Trapezocapitate ligament)
- Palmar capitotrapezoid ligament (Trapezocapitate ligament)
- Trapeziotrapezoid ligament
- Dorsal trapeziotrapezoid ligament
- Palmar trapeziotrapezoid ligament
- Capitohamate ligament
- Volar capitohamate ligament
- Dorsal capitohamate ligament
- Dorsal deltoid ligament
- Anterior oblique ligament (beak ligament)
- Flexor retinaculum of wrist
- Extensor retinaculum of wrist
- Palmar aponeurosis
- Triangular fibrocartilage complex (TFCC )
- Triangular fibrocartilage disc
- Radialis indicis artery
- Princeps pollicis artery
- Dorsal carpal branch of radial artery
- Superficial palmar arch
- Deep palmar arch
- Palmar branch of cephalic vein
- Perforating branches of ulnar veins
- Dorsal venous network of hand
- Deep venous palmar arch
- Deep branch of ulnar nerve
- Dorsal digital branches of radial nerve
- Dorsal digital branch of ulnar nerve
- Common palmar digital branch of ulnar nerve
- Common palmar digital nerves of median nerve
- Proper palmar digital nerves
- Guyon’s canal
- Phalanx bone (hand)
- Proximal phalanx of hand
- Middle phalanx of hand
- Distal phalanx of hand
- Head of the phalanx (hand)
- Base of the phalanx (hand)
- Body of the phalanx (hand)
- Second dorsal interosseous muscle of hand
- Dorsal interosseous muscle of hand
- Palmar interosseous muscles of hand
- Metacarpophalangeal joints
- Proximal interphalangeal joints of hand
- Distal interphalangeal joint of hand
- Tuberosity of distal phalanx
- Olfactory trigone
- Olfactory tubercle
- Ophthalmic nerve
- Lesser wing of sphenoid
- Anterior clinoid process
- Sphenoparietal sinus
- Carotid siphon
- Scala vestibuli
- Scala media
- Scala tympani
- Interscalar septum
- Spiral canal of cochlea
- Cochlear duct
- Utricle
- Saccule
- Posterior semicircular canal
- Lateral semicircular canal
- Anterior semicircular canal
- Posterior bony ampulla
- Common bony crus
- Mastoid air cells
- Cochlear Canaliculus
- Inferior vestibular nerve
- Superior vestibular nerve
- Tympanic segment of facial nerve
- Temporal lobe
- Anterior bony ampulla
- Apex of insula
- Insular lobe
- Genioglossus muscle
- Nasal bones
- Ascending pharyngeal artery
- Medial atlantoaxial joint
- Pharyngeal tonsil
- Frontal bone
- Hard palate
- Frontal sinus
- Ethmoid sinus
- Ethmoidal air cells
- Sphenoid sinus
- Middle Nasal Meatus
- Inferior nasal meatus
- Superior nasal meatus
- Central axillary lymph nodes
- Right lung
- Left lung
- Retrosternal space
- Manubriosternal joint
- Jugular notch
- Clavicular notch
- Sternal angle
- Anterior sternoclavicular ligament
- Xiphisternal joint
- Radiate sternocostal ligament
- Jugular tubercle
- Intervertebral foramen
- Groove for vertebral artery
- Apical ligament of dens
- Superior pharyngeal constrictor muscle
- Middle pharyngeal constrictor muscle
- Inferior pharyngeal constrictor muscle
- Periaortic lymph nodes
- Middle Colic Vein
- Posterior cecal artery
- Ampulla of vas deferens
- Deep dorsal vein of penis
- Internal pudendal artery
- Internal pudendal vein
- Ureteric Orifice
- Lateral fornix of cervix
- Posterior fornix of cervix
- Anterior fornix of cervix
- Posterior glenoid labrum
- Anterior glenoid labrum
- Transverse humeral ligament
- Deep brachial artery
- Articular facet of head of radius
- Cubital anastomosis
- Nail (hand)
- Nail bed (hand)
- Nail bed corion (hand)
- Lateral nail fold (hand)
- Adipose tissue (hand)
- Dermis of skin (hand)
- Epidermis of skin (hand)
- Volar plate (hand)
- Interosseous lateral band
- Flexor tendon synovial sheath
- Central slip of common extensor tendon
- Dorsal interossei tendon hand
- Palmar Interossei Tendon hand
- Dorsal digital nerve (hand)
- Proper palmar digital nerve (hand)
- Proper palmar digital arteries (hand)
- Proper palmar digital veins (hand)
- Dorsal digital veins (hand)
- Dorsal digital arteries (hand)
- Dorsal capsule of the metacarpophalangeal joint
- Proper collateral ligament
- Accessory collateral ligament
- Annular ligament (annular pulley)
- Head of distal phalanx
- Base of distal phalanx
- Intermediate phalanx
- Head of proximal phalanx
- Body of proximal phalanx
- Base of proximal phalanx
- Acetabular notch
- Trochanteric fossa
- Posterior wall of acetabulum
- Anterior wall of acetabulum
- Gluteal tuberosity
- Third trochanter
- Intertrochanteric crest
- Crista galli
- Lacrimal bone
- Septum of sphenoid sinus
- Eyeball
- Vertebral artery
- Right coronary aortic sinus
- Left coronary aortic sinus
- Straight Arteries
- Right branch of portal vein
- Left branch of portal vein
- Anterior right branch of portal vein
- Posterior right branch of portal vein
- Annular ligaments (annular pulleys)
- Basilar part of pons
- Basilar venous plexus
- Cerebellar falx
- Inferior hemispheric cerebellar veins
- Lateral part of biventeral lobule
- Medial part of biventeral lobule
- Medullopontine sulcus
- Peduncle of flocculus
- Pontomedullary junction
- Preolivary groove
- Pyramid of medulla oblongata
- Retroolivary groove
- White substance of cerebellum
- Pontine artery
- Anterolateral pontine vein
- Superior hemispheric cerebellar veins
- Crus cerebri
- Tegmentum of pons
- Superior cerebellar peduncle
- Posterior quadrangular lobule
- Vermis of cerebellum
- Amygdalohippocampal area
- Infundibulum
- Anterior calcarine sulcus
- Rostral gyrus
- Rostral sulcus
- Orbital Sulci
- Orbital gyri
- Paraolfactory sulci
- Posterior orbital sulcus
- Transverse occipital sulcus
- Transverse temporal sulcus
- Hypothalamus
- Extreme capsule
- foramen of Monro
- Cerebral falx
- Meninges
- Frontobasal artery
- Inferior parietal lobule
- Body of lateral ventricle
- Perivascular spaces
- Paracentral lobule
- Paracentral gyrus
- Marginal branch of cingulate sulcus
- Sagittal suture
- Posterior median sulcus of medulla oblongata
- Pons (basilar portion)
- Medial lemniscus
- Spinothalamic tract
- Gracile fasciculus
- Cuneate fasciculus
- Hypoglossal nucleus
- Dorsal nucleus of vagus nerve
- Nucleus of the solitary tract
- Spinal trigeminal nucleus (pars caudalis)
- Spinal trigeminal nucleus (pars oralis)
- Spinal trigeminal nucleus
- Ventral cochlear nucleus
- Dorsal cochlear nucleus
- Nucleus supraspinalis
- Pontocerebellar fibers
- Parabrachial recess
- Lateral lemniscus
- Spinal lemniscus
- Fibers of trigeminal nerve
- Principal sensory nucleus of trigeminal nerve
- Locus ceruleus
- Nucleus reticularis tegmenti pontis
- Pes hippocampi
- Hypophysial cistern
- Amygdaloclaustral area
- Lateral pallidum
- Medial pallidum
- Caudatolenticular gray bridges
- Hypothalamic sulcus
- Lateral groove of midbrain
- Tectal plate
- Precommunicating part of posterior cerebral artery
- Calcarine branch of posterior cerebral artery
- Tenia of fornix
- Stria medullaris thalami
- Habenula
- Tela choroidea of third ventricle
- Choroid plexus of the lateral ventricle
- Medial vein of lateral ventricle
- Vertex
- Coronal suture
- Lambdoid suture
- Frontal suture
- Parietal bone
- Temporal bone
- Nasal bone
- Maxillary bone
- Zygomatic process of frontal bone
- Frontal process of zygomatic bone
- Petrous ridge
- Orbital cavity
- Medial wall of orbit
- Lateral wall of the orbit
- Supraorbital margin
- Infraorbital margin
- Sphenoidal sinus
- Lateral wall of maxillary sinus
- Medial wall of maxillary sinus
- Inferior wall of maxillary sinus
- Superior wall of the maxillary sinus
- Bony nasal septum
- Perpendicular plate
- Cribriform plate
- Nasal crest of maxilla
- Teeth
- Angle of mandible
- Coronoid process of mandible
- Superciliary arch
- Innominate line (skull)
- Internal occipital crest
- Odontoid process
- Nasal part of frontal bone
- Frontonasal suture
- Anterior ethmoidal air cells
- Nasal spine of frontal bone
- Alveolar arch of maxilla
- Cartilaginous part of nasal septum
- Lateral nasal cartilage
- Major alar cartilage
- Minor alar cartilage
- Apex of nose
- Apex of right lung
- Apex of left lung
- Superior lobe of right lung
- Superior lobe of left lung
- Middle lobe of right lung
- Inferior lobe of right lung
- Inferior lobe of left lung
- Base of right lung
- Hilum of lung
- Aortic knob
- Mediastinum
- Right paratracheal stripe
- Left paratracheal stripe
- Right paraspinal line
- Left paraspinal line
- Paraaortic line
- Azygoesophageal line
- Right cardiophrenic angle
- Left cardiophrenic angle
- Right costophrenic angle
- Left costophrenic angle
- Glenohumeral joint
- Head of rib
- Neck of rib
- Body of rib
- Anterior ribs
- Posterior ribs
- Intercostal space
- Gastric bubble
- Breast shadow
- Axilla
- C1 Vertebra (Atlas)
- C2 Vertebra (Axis)
- Zygapophyseal joint
- Uncinate process of vertebra
- Intervertebral disc space
- Aortic arch
- Annular epiphysis
- Sacrococcygeal joint
- Iliac bone
- Iliac fossa
- L (Lumbar spine)
- S (Sacral spine)
- Co (Coccyx)
- T (Thoracic spine)
- C (Cervical spine)
- Fovea for ligament of head of femur
- Obturator foramen
- Transverse abdominal muscle
- Superior articular process of sacrum
- Penis
- Hamstring muscles
- Shenton’s line
- Iliopectineal line
- Ilioischial line
- Adductor tubercle
- Intercondylar fossa
- Articular surface of medial femoral condyle
- Articular surface of lateral femoral condyle
- Groove for popliteus muscle
- Medial condyle of tibia
- Lateral condyle of tibia
- Intercondylar eminence
- Articular surface of medial tibial condyle
- Articular surface of lateral tibial condyle
- Fibular articular facet of tibia
- Body of fibula
- Apex of head of fibula
- Articular facet of head of fibula
- Lateral tibiofemoral joint space
- Medial tibiofemoral joint space
- Tubercle of iliotibial tract
- Lateral supracondylar line
- Medial supracondylar line
- Superior rim of acetabulum
- Anterior rim of acetabulum
- Posterior rim of acetabulum
- Inferior rim of acetabulum
- Inferior articular surface of tibia
- Fibular notch of tibia
- Inferior tibiofibular joint
- Posterior malleolus
- Apex of medial malleolus
- Apex of lateral malleolus
- Articular facet of lateral malleolus
- Articular facet of medial malleolus
- Anterior colliculus of medial malleolus
- Posterior colliculus of medial malleolus
- Malleolar fossa
- Trochlea of talus
- Superior facet of talus
- Medial malleolar facet of talus
- Lateral malleolar facet of talus
- Calcaneal tuberosity
- Medial process of calcaneal tuberosity
- Lateral process of calcaneal tuberosity
- Calcaneal tubercle
- Subtalar joint
- Talonavicular joint
- First intercuneiform joint
- Second intercuneiform joint
- Tuberosity of fifth metatarsal bone
- Metatarsal Bones (MT)
- Kager’s fat pad
- Tuberosity of cuboid bone
- Tarsal sinus
- Articular surface for cuboid bone
- Tuberosity of distal phalanx of foot
- Trochlea of phalanx
- Metatarsophalangeal joint of great toe
- Interphalangeal sesamoid of great toe
- Tuberosity of first metatarsal bone
- Intermetatarsal joints
- Lisfranc complex
- Navicular articular surface
- Cuboid articular surface
- Body of distal phalanx of great toe
- Head of distal phalanx of great toe
- Base of distal phalanx of great toe
- Tuberosity of distal phalanx of great toe
- Trochlea of phalanx of great toe
- Base of proximal phalanx of great toe
- Body of proximal phalanx of great toe
- Head of proximal phalanx of great toe
- Head of first metatarsal bone
- Body of first metatarsal bone
- Base of first metatarsal bone
- Second tarsometatarsal joint
- First tarsometatarsal joint
- Posterior talar articular surface
- Middle talar articular surface
- Fibular trochlea
- Anterior talar articular surface
- Lateral tubercle of talus
- Posterior calcaneal articular facet
- Soleal line
- Superior tibiofibular joint
- Posterior process
- Medial tubercle of talus
- Lateral process of talus
- Tibiofemoral joint space
- Trapezoid Line
- Superior border of scapula
- Medial border of scapula
- Lateral border of scapula
- Superior angle of scapula
- Inferior angle of scapula
- Anterior rim of glenoid
- Posterior rim of glenoid
- Supraglenoid tubercle
- Infraglenoid tubercle
- Crest of greater tubercle
- Crest of lesser tubercle
- Radial fossa
- Tuberosity of ulna
- Body of ulna
- Lateral border of humerus
- Medial border of humerus
- Metacarpophalangeal joint of thumb
- Ulnar sesamoid bone of thumb
- Radial sesamoid bone of thumb
- Intermetacarpal joints
- Carpometacarpal joint of thumb
- Tubercle of scaphoid
- Interosseous border
- Body of distal phalanx
- Head of middle phalanx
- Body of middle phalanx
- Base of the middle phalanx
- Interphalangeal joint of thumb
- Base of middle phalanx
- Sesamoid bone of interphalangeal joint
- Proximal phalanx of thumb
- Metacarpal bone of thumb
- Posterior clinoid process
- Pituitary fossa
- Soft palate
- Posterior nasal spine
- Posterior part of tongue
- Superior wall of orbit
- Glabella
- Frontal process of maxilla
- Mental protuberance
- Mandibular notch
- Posterior border of maxilla
- Incisive foramen
- Floor of the maxillary sinus
- Medial wall of the maxillary sinus
- Pterygomaxillary fissure
- Floor of orbit
- Infraorbital canal
- Nasal cavity
- Apical foramen
- Periodontal ligament
- Cementum
- Dental pulp
- Cementoenamel junction
- Dentine
- Enamel
- Tibial shaft

The exiting nerve root refers to the ventral and dorsal root fibers that join to form a spinal nerve as it leaves the spinal canal through the intervertebral foramen. Each spinal segment gives rise to a pair of spinal nerves (31 pairs in total: 8 cervical, 12 thoracic, 5 lumbar, 5 sacral, and 1 coccygeal). The exiting root carries both motor and sensory fibers and is a common site of compression in spinal degenerative disease, disc herniation, trauma, or tumors.
Synonyms
-
Spinal nerve exiting root
-
Intervertebral foramen nerve root
-
Peripheral spinal root
Origin, Course, and Exit
-
Origin: Arises from union of dorsal (sensory) and ventral (motor) roots at the spinal cord
-
Course:
-
Travels laterally within the dural sleeve
-
Passes through the lateral recess and intervertebral foramen
-
Surrounded by fat and bordered by pedicles, vertebral body, and facet joint
-
-
Exit: Leaves the vertebral canal via the intervertebral foramen to join the peripheral nerve plexuses
Relations
-
Anteriorly: Vertebral body, intervertebral disc, uncovertebral joint (cervical), posterior longitudinal ligament
-
Posteriorly: Lamina and ligamentum flavum
-
Superiorly/Inferiorly: Pedicles of vertebra above and below
-
Laterally: Paravertebral muscles and sympathetic chain
Function
-
Transmits motor fibers to skeletal muscles
-
Transmits sensory fibers from skin, joints, and muscles to CNS
-
Carries autonomic fibers to peripheral targets
-
Serves as a pathway for reflex arcs and voluntary movement
Clinical Significance
-
Common site of compression from disc herniation, spondylosis, ligament hypertrophy, or foraminal stenosis
-
Responsible for classic radicular pain syndromes (sciatica, cervical radiculopathy)
-
Target for nerve root blocks, steroid injections, and surgical decompression
-
Important in tumor evaluation (schwannomas, neurofibromas)
MRI Appearance
T1-weighted images:
-
Exiting nerve roots appear as linear low-to-intermediate signal structures
-
Surrounded by bright fat in the intervertebral foramen
T2-weighted images:
-
Nerve roots show intermediate to mildly hyperintense signal compared to muscle
-
Pathological nerve root compression, edema, or neuritis: brighter signal intensity
STIR (Short Tau Inversion Recovery):
-
Normal nerve root: low signal
-
Inflamed or compressed nerve root: bright hyperintensity
-
Surrounding fat suppressed to highlight pathology
T1 Fat-Sat Post-Contrast:
-
Normal nerve root enhances minimally or not at all
-
Pathologic root (neuritis, tumor, infection) shows focal or diffuse enhancement
3D T2 SPACE / CISS:
-
Nerve roots appear as intermediate to mildly hyperintense signal compared to muscle
-
Surrounded by very bright CSF, providing excellent contrast
-
Ideal for detecting root compression, tethering, or small intradural lesions
CT Appearance
Non-Contrast CT:
-
Nerve roots not directly seen but inferred within foramina
-
Foramen appears widened or narrowed in pathology
-
Herniated disc or osteophytes impinging on the root can be identified
Post-Contrast CT (CT Myelography):
-
Nerve roots outlined by contrast-filled CSF
-
Compression or displacement is visible as root sleeve cut-off, irregularity, or filling defect
-
Helpful in patients with MRI contraindications
MRI image
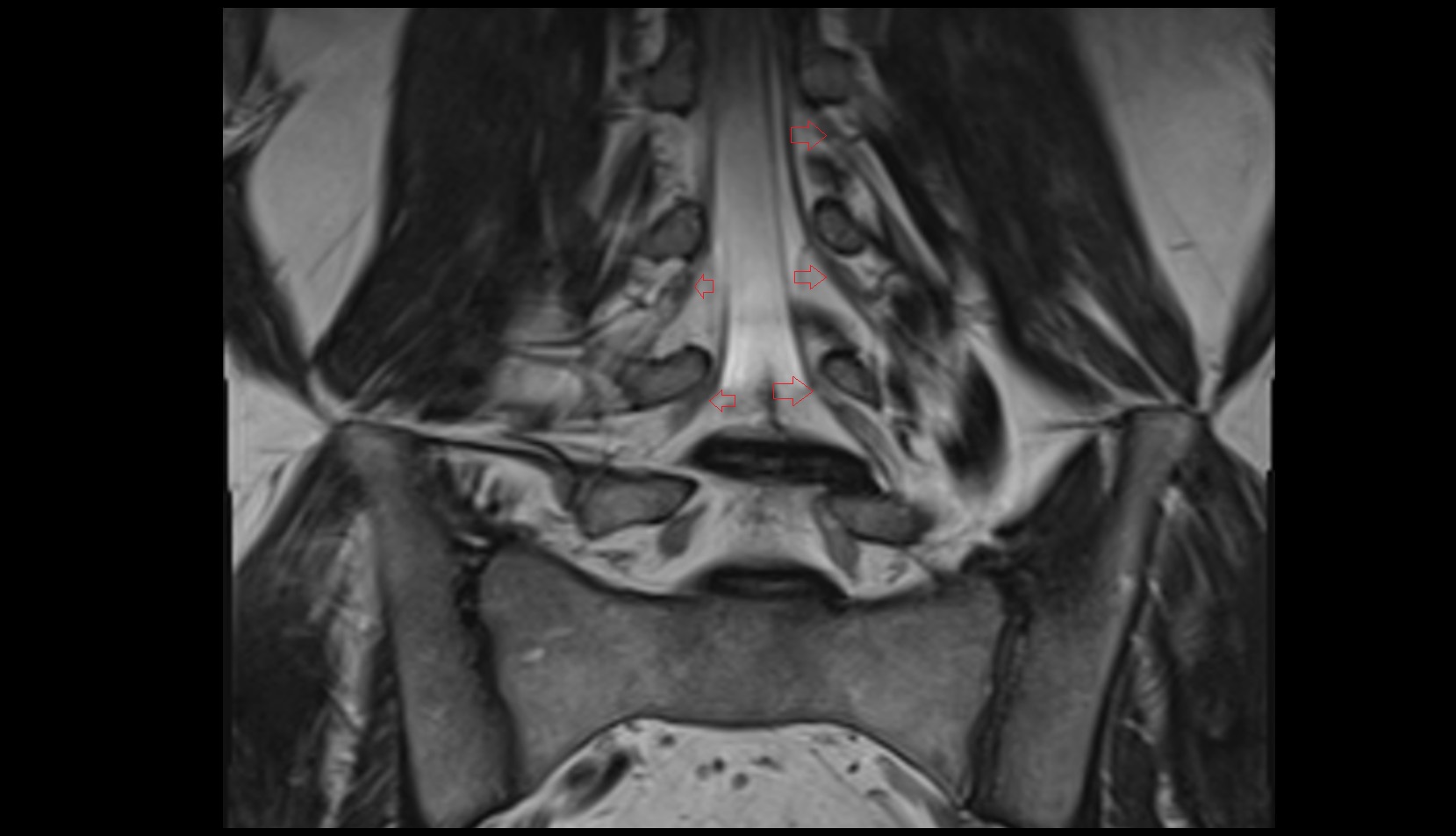
MRI image
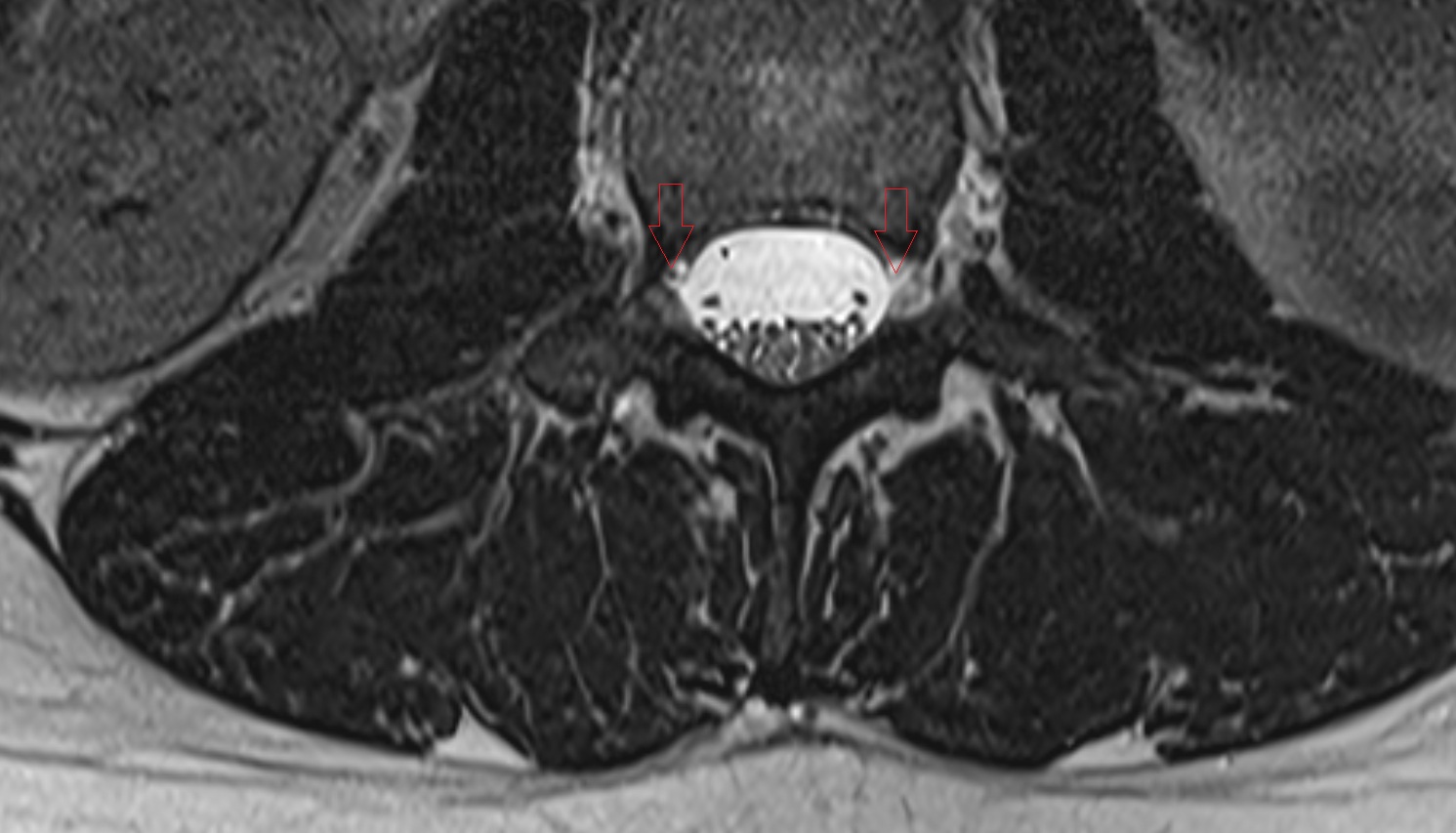
MRI image
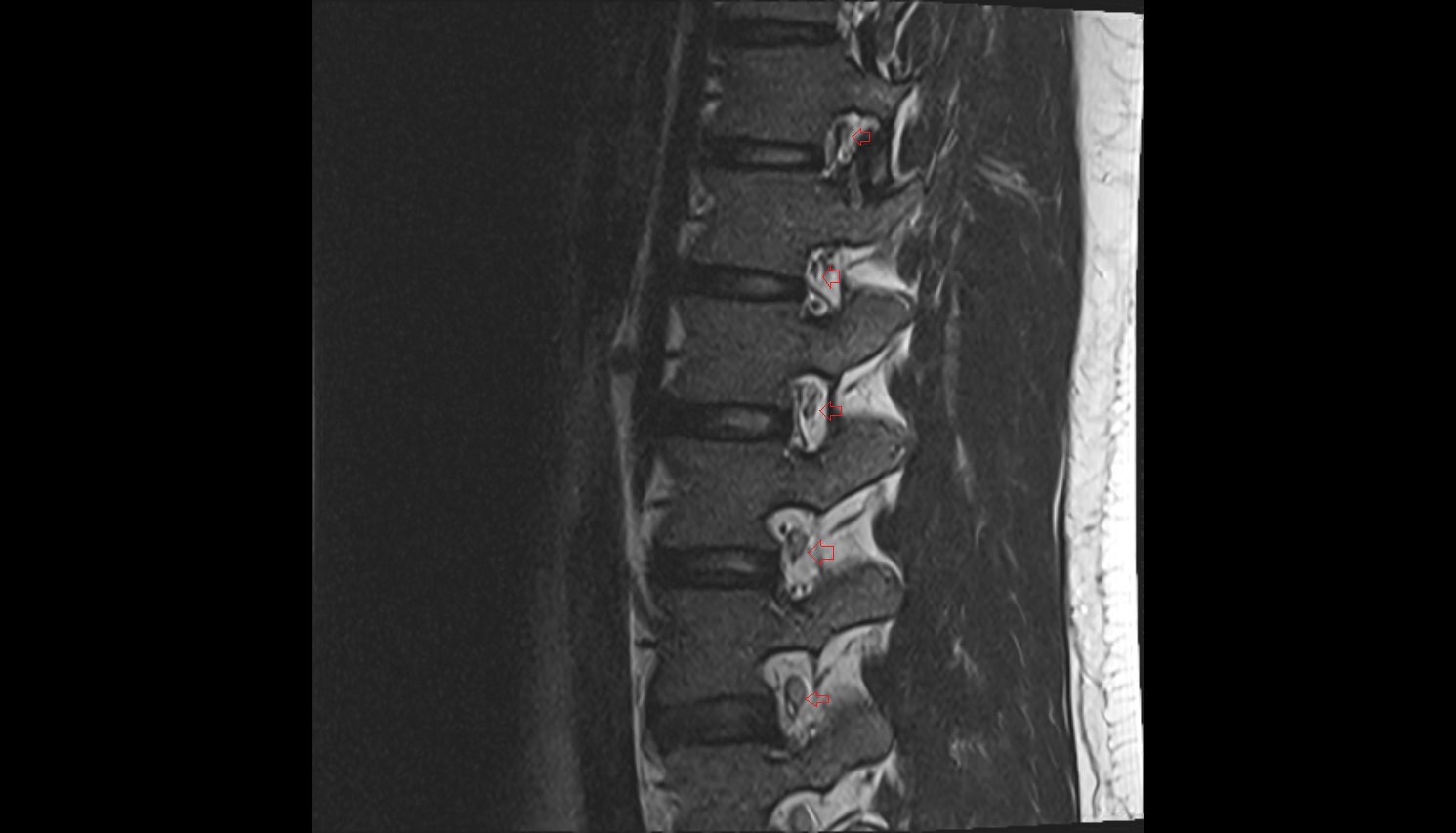
MRI image
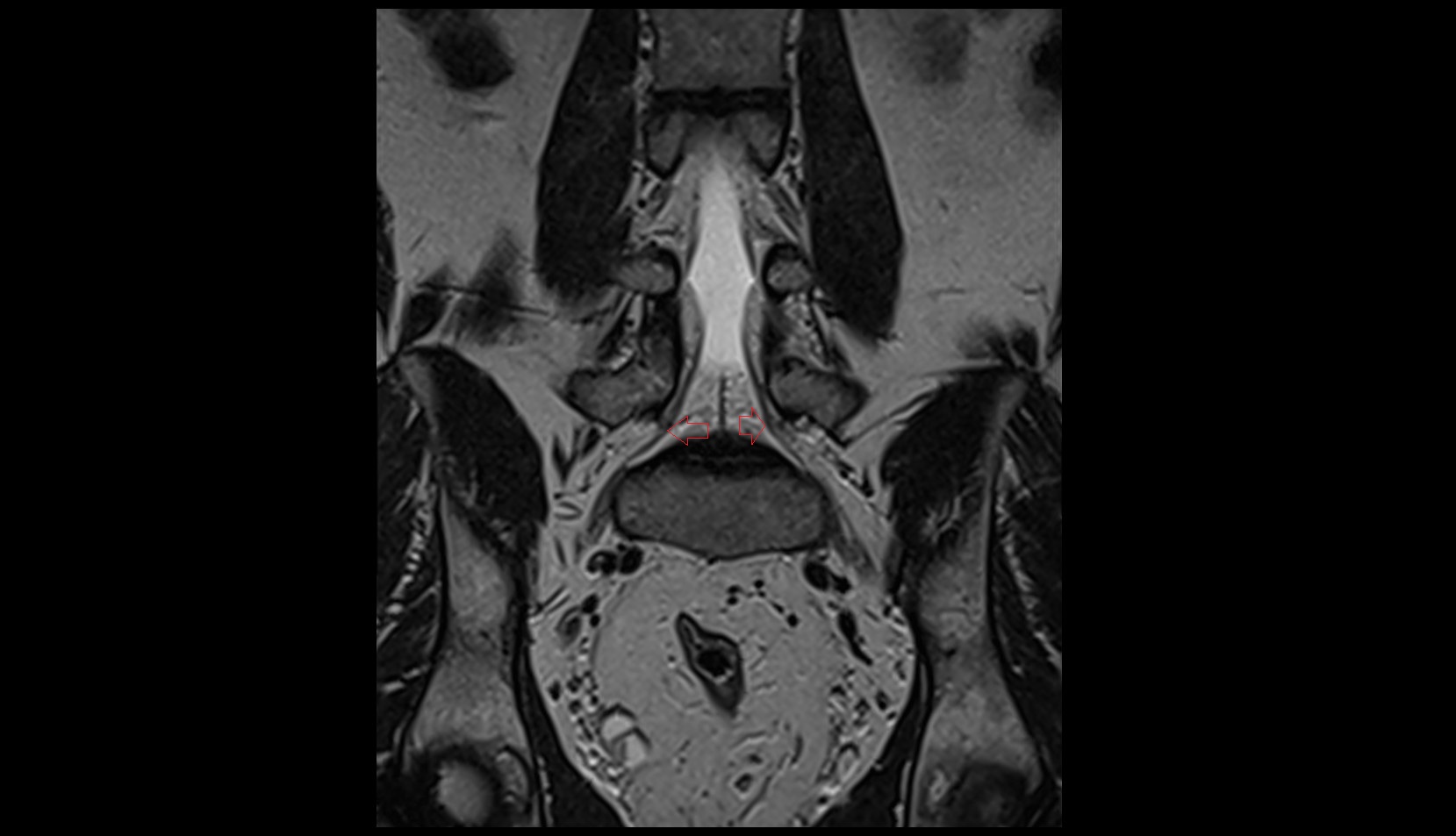
CT image